If you see many geriatric patients, there is no doubt you see a lot of macular issues. There is a lot of confusion among patients and families of the patients between wet and dry macular degeneration. In fact, some think that wet macular degeneration is a better diagnosis to have since laser surgery can be performed. That is incorrect. This article will explain what the macula is, where it is located in the eye, the difference between dry and wet macular degeneration, and the treatments for both conditions.
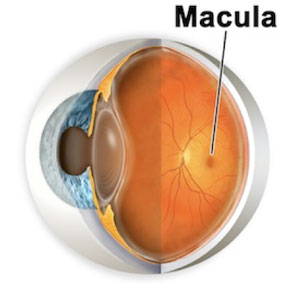 The macula lutea of the retina is an oval- shaped pigmented area near the center of the retina of the human eye. (Macula means spot in Latin, lutea meaning yellow.) It has a diameter of around 5.5mm. The macula is subdivided into the umbo, foeola, foveal avascular zone, fovea, para-fovea, and peri-fovea areas. The fovea is located near the center of the macula. It is a small pit that contains the largest concentration of cone cells. The retina contains two different types of photosensitive cells, the rod cells and the cones. These cells make the macula responsible for the central, high resolution, color vision that is possible in good light and this kind of vision is impaired if the macula is damaged, in cases as macular degeneration.
The macula lutea of the retina is an oval- shaped pigmented area near the center of the retina of the human eye. (Macula means spot in Latin, lutea meaning yellow.) It has a diameter of around 5.5mm. The macula is subdivided into the umbo, foeola, foveal avascular zone, fovea, para-fovea, and peri-fovea areas. The fovea is located near the center of the macula. It is a small pit that contains the largest concentration of cone cells. The retina contains two different types of photosensitive cells, the rod cells and the cones. These cells make the macula responsible for the central, high resolution, color vision that is possible in good light and this kind of vision is impaired if the macula is damaged, in cases as macular degeneration.
Many people develop macular degeneration as a part of the body’s natural aging process. Hence the term, Age Related Macular Degeneration or ARMD. With ARMD the symptoms are blurriness, dark areas or distortion in your central vision, and perhaps permanent loss of your central vision. It doesn’t normally affect peripheral vision.
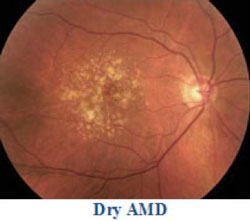
Dry AMD is the most common type of macular degeneration affecting 90% of the people who have macular degeneration. The dry form of macular degeneration is a breakdown or thinning of the layer of the retinal pigment epithelial cells in the macula. These cells support the light-sensitive photoreceptor cells that are critical to vision. The photoreceptors gather the images and send them to the brain, where vision takes place. The death of these cells is called atrophy. Dry macular degeneration can reduce the central vision and affect color perception. This damage is not severe and doesn’t decrease vision as rapidly as the wet form of macular degeneration. Many doctors recommend using AREDS supplements to protect your eyes from the sun, to eat fruits and vegetables and fish due to the amount of omega-3.
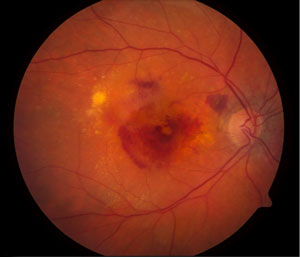
Wet Macular Degeneration
Wet macular degeneration is a more advanced type of macular degeneration. Wet macular degeneration affects only 10-15% of patients, although it accounts for 90% of severe vision loss caused by macular degeneration. The membrane underlying the retina thickens and then breaks. The oxygen supply to the macula is disrupted and the body responds by growing new, abnormal blood vessels. These vessels grow behind the retina raising it. These vessels are fragile and can leak and of most concern is that the vessels can grow behind the retina raising it and causing it to detach. This can cause scarring and damage the macula. Once this vision is destroyed, it cannot be repaired. The treatment for wet Macular degeneration is laser surgery.
With the increase of geriatric patients, you will see these conditions more frequently in your office. Be prepared to do referrals to a Retinal Specialist. Also, be aware of the issues patients may have after the diagnosis and treatments of these conditions. The patient’s correctable visual acuity may be limited. The patients need to be educated about their diagnosis and given the information for follow-up care.
Information received from aao.org

Linda Hardy received the American Optometric Association Paraoptometric of the Year Award at the 2016 SECO meeting in Atlanta, Georgia. Linda is a Certified Optometric Technician (COT) and Certified Ophthalmic Assistant (COA). She is also ABO and NCLE certified and a Licensed Dispensing Optician (LDO) in the state of Georgia.
A graduate of Georgia Medical Institute as a Registered/ Certified Medical Assistant, Linda began her optical career working with a group of ophthalmologists as an ophthalmic assistant. She has been the Clinical Coordinator with a private optometry practice in Newnan, Georgia for 15 years.
Linda is also a speaker and educator at regional optical meetings. She and her husband have five children, and she enjoys spending time with her family, exercising, reading and volunteering in her community.













