Unleash the Power of the Corridor
By Barry Santini, ABOM
Release Date: September 15, 2022
Expiration Date: May 18, 2023
Learning Objectives:
Upon completion of this program, the participant should be able to:
- Explain how free form progressive designs improve overall design flexibility over conventional progressive lenses.
- Describe the factors that help in a corridor length specification. including Rx, frame fit and patient posture.
- List the major reference points on a progressive lens and describe their purpose.
Faculty/Editorial Board
 Barry Santini graduated from New York Technical College in 1975 with an AAS in Ophthalmic Dispensing. He is a New York State licensed optician with contact lens certification, is ABO certified and was awarded an ABO Master in 1994. As sales manager for Tele Vue Optics from 1987 to 2003, Santini developed his knowledge of precision optics and has been an owner of Long Island Opticians in Seaford N.Y. from 1996 to present. In addition, Santini is an amateur astronomer and lecturer and plays bass trombone in the Brooklyn Symphony.
Barry Santini graduated from New York Technical College in 1975 with an AAS in Ophthalmic Dispensing. He is a New York State licensed optician with contact lens certification, is ABO certified and was awarded an ABO Master in 1994. As sales manager for Tele Vue Optics from 1987 to 2003, Santini developed his knowledge of precision optics and has been an owner of Long Island Opticians in Seaford N.Y. from 1996 to present. In addition, Santini is an amateur astronomer and lecturer and plays bass trombone in the Brooklyn Symphony.
Credit Statement
This course is approved for one (1) hour of CE credit by the American Board of Opticianry (ABO) for Technical Ophthalmic Level 2. Course # STWJHI061-2
This course is intended to help opticians maximize success with free form progressive lenses. The 21st century dispenser has new freedoms to tailor progressive lenses to the individual, customizing them to meet the patients’ specific vision needs. Choosing the corridor length best suited to the “postural habits and vision tasks” is one of the most impactful ways a dispenser can contribute to the best vision for progressive lens patients.
2022 marked the 25th anniversary of direct-to-lens sur facing, free form technology for manufacturing progres sive lenses. Seiko was the initial holder of the patent for FreeForm® technology; their lens was the P1 progressive, and the year was 1997. (The patent has since expired.) Over two decades have passed, yet eyecare professionals still struggle to fully understand all the salient advantages of free form lenses and how to tailor a progressive design to the wearer’s needs. The origins of this struggle lie in our intrinsic human nature to reject change. Hence, many ECPs still approach progressive lens fitting by start ing with frames with deep B dimensions to facilitate lon ger corridors and fitting heights. This fitting approach was acceptable in the era of molded front surface designs leading up to the early 2000s. But today, free form technology allows far more flexibility and customization for knowledgeable opticians to utilize in creating person alized lenses designed to optimize the lens and deliver the best optics to meet the needs of the wearer.
Let’s begin with a review of the history of progressive lens designs.
PROGRESSIVE DESIGN: THE PAST
During the first 25 years of progressive lenses, both professionals and the public were at the mercy of whatever front-molded design paradigm was the flavor of the day for a specific brand progressive lens. For example, Varilux 2 featured a single mono design that was scaled as the add power increased. Different Varilux designs followed from Infinity to Panamic to Varilux Comfort, and each one promised improved performance and wearer comfort through each lens’ new approach to balancing progressive design. Other lenses, such as American Optical’s Omni, sought to dramatically lower the amplitude of surface astigmatism by spreading its gradient, literally across the entire surface, using an approach referred to as bi-polar design.
Meanwhile, Sola’s VIP found a legion of satisfied wearers with its hard design, which featured improved near utility in its large and easily accessed reading area, also known as a shorter corridor. In the meantime, other manufacturers, ZEISS for example, was the first company to address the impact of asymmetric astigmatism by managing it in a binocularly-optimized and symmetrically-weighted design called Gradal HS—for horizontal symmetry. But no matter the theoretical approach used, significant trade-offs were common in progressives made with a molded front-surface design.
PROGRESSIVE DESIGN: THE PRESENT
Almost by magic, the advent of free form, aspherical lens production technology gave designers and dispensers the ability to tailor various aspects of progressive design to a patient’s individual vision needs. For example, the design can be optimized to minimize aberrations based on the fitting parameters, biometrics and the Rx, resulting in wider fields of view. In addition, choosing the ideal lens corridor length facilitates easy access to the lens’ distance, intermediate, and near areas. Therefore, selecting the progressive corridor length becomes an important responsibility for the dispenser.
PROGRESSIVE DESIGN: THE FUTURE
Beyond taking the personal position of wear measurements, future assessment technologies will provide comprehensive and precise quantification of a full suite of individual biometric data, including but not limited to:
1. Precise Center of Rotation (CoR) data: By knowing, rather than estimating, the exact center of rotation of an individual’s eyes, opticians in the future can facilitate superior optimization of peripheral lens performance.
2. Axial length: Large data banks of biometric data in the future will result in the ability to produce more accurate default values for axial length, an important factor in determining the precise CoR.
3. Eye rotation data: This information intrinsically impacts corridor placement and length. Individually ascertained eye rotation data—both in horizontal and vertical directions—is used to determine optimal corridor length and placement, allowing the design to be tailored for differing activities.
The more data gathered regarding the precise CoR for a large population of eyes, the better the default averages extrapolated. In addition, the more complete our understanding of the relationships between prescription, corneal curvature, crystalline lens power and axial length allows for better biometrically optimized designs.
HUMAN VISION PLASTICITY
One of human vision’s most significant advantages—it is inherently adaptable. Our brain can adapt and function amazingly well relative to our visual system despite less-than-optimal conditions, such as eyewear made off-spec or with optically poor performing materials or incorrect centration. Unfortunately, this adaptability can also mask the suboptimal performance of lenses. Interestingly, the ophthalmic field generally points to the human eye exhibiting a “just noticeable difference,” or JND of 0.12 diopters. This translates to an optical path difference at the retinal plane of 0.04 mm. The human eye is therefore, a marvel of optical engineering, able to keenly detect minimal differences in focus while simultaneously tolerating and adapting to prescriptions as much as 0.50 diopter off optimum focus— a number four times the JND at the retinal plane.
Given the brain’s ability to compensate and adapt to ophthalmic lenses, our ability to evaluate whether the lens is providing the patient with optimal vision can be elusive. Just because patients adapt to suboptimal lenses doesn’t mean we don’t strive to deliver optimal lenses every time. For this reason, a comprehensive understanding of how progressive design can be individually tailored to optimize lens performance is the essential skill of the 21st century optician.
UNDERSTANDING PROGRESSIVE BASICS
The authors of Modern Ophthalmic Optics, Jose Alonso et al., tell us that ECPs who want better control of the selection of progressive designs should be aware of not just the MFH but also indicators about the start of the progression. They go on to say that knowledge of three values, the PRP, MFH and the Corridor length of the design, will provide the ECP with the essential details that influence the progressive design performance.
PAL MAJOR REFERENCE POINTS DEFINITION
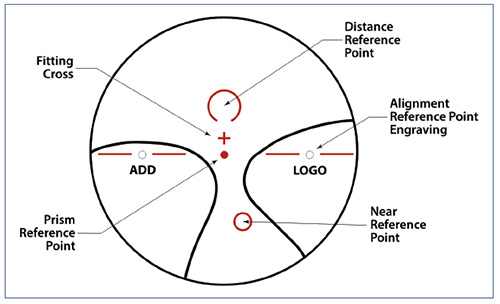 Fitting Point: The reference point for the progressive design’s fitting cross location. The common
orthodoxy is to place the fitting point at the center
of the eye’s pupil, while the patient’s facial plane is
in its natural position, i.e., normal posture. This
point on the lens is for correct centration as it is
intended to align with the wearer’s visual axis.
Fitting Point: The reference point for the progressive design’s fitting cross location. The common
orthodoxy is to place the fitting point at the center
of the eye’s pupil, while the patient’s facial plane is
in its natural position, i.e., normal posture. This
point on the lens is for correct centration as it is
intended to align with the wearer’s visual axis.
Most commonly, the progressive lens corridors’ power profile begins its slope at the fitting point, and the distance and near areas are prioritized. Lens designers do this to smooth the transition between distance and intermediate areas, and it is one of the reasons why the distance reference point (DRP) is kept 6 mm or more above the fitting point. In most general-purpose designs, the add power progression is slow and gradual for the first 2 to 4 mm below the fitting point.
According to the Minkwitz theorem, surface astigmatism lateral to the corridor increases the quicker the add power progression builds and the higher the add power. Therefore: Rate of Change in Power = Add Power ÷ Corridor Length. Although free form technology optimizes the surface to minimize surface astigmatism lateral to the umbilic (the center line of the corridor), there are mathematical/geometrical limits to the amount of reduction possible.
Distance Reference Point (DRP): The area located 6 mm above the fitting point is used for verifying the distance prescription. We do not verify the distance Rx at the fitting point because many lens designs start their progressive slope, although very gradually at this point. This fact is why progressive lenses are acutely more sensitive to how properly calibrated the distance Rx is for sharp driving vision.
Prism Reference Point (PRP): The PRP is the specified point for measuring the prescribed prism or prism thinning in a progressive lens. The textbook definition of this point on a progressive lens is the major reference point (MRP) unless a prism is present, and then it is the point on the lens used to verify the prism. The terms are interchangeable. The PRP is located centrally between the alignment reference engraved markings. This is the lens designer’s point of reference for optical calculations and lens alignment.
Alignment Reference Markings: Also known as the alignment engravings, they are positioned 34 mm apart, 17 mm from the center PRP and at the same height as the PRP. These engravings are used for verifying the correct axis alignment of the progressive lens and for marking and remarking the lens for finishing and final lens verification. The add power is indicated under the temporal engraving.
Near Reference Point (NRP): The area designated for verifying the reading Rx power.
FITTING CONCEPTS
Below are the definitions and fitting concepts to help ECPs fully grasp the mechanics of choosing corridor length:
Corridor Length: The linear distance between the beginning of the power gradient, the Fitting Point and the target add value.
Corridor Target Add Value: Variably defined by the lens manufacturer for individual designs and typically falls at a point on the lens between 85 and 100 percent of the prescribed add value. Manufacturers are free to define corridor lengths using a different percentage of add as the target value. Know the designs you work with and ask the manufacturer what target value they use when defining their corridor length. If you want to compare corridor lengths between designs, the rule of thumb: Add approximately 2 mm to the corridor length of an 85 percent target add value design when comparing corridor lengths with a 100 percent target value design.
Minimum Reading Area: Experience has shown that a progressive reading area less than 5 mm in height is undesirable.
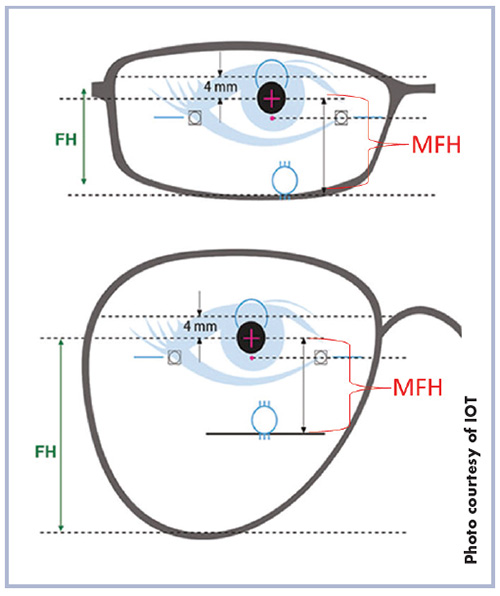
Minimum Fitting Height (MFH): Lens manufacturers provide minimum fitting height values for their designs. Generally, MFH is the distance from the fitting point to the near reference point, plus a minimum allowance of 4 mm. A general recommendation is to choose a frame that would allow the addition of 4 mm allowance to the MFH to ensure the full reading utility is available for the wearer and avoid truncation of part of the reading area. Note: The corridor length is based on the MFH. You can choose from the design’s corridor length options; otherwise, the design’s internal algorithm automatically chooses a corridor length.
 RULE OF THUMB FOR
CORRIDOR LENGTH SELECTION
RULE OF THUMB FOR
CORRIDOR LENGTH SELECTION
To determine the desired corridor length, I recommend starting with the minimum fitting height and adding 5 mm to ensure a functional reading area. The minimum fitting height, less 5 mm, is a good approximation for a target corridor length. For example, let’s say you have a minimum fitting height of 18 mm; a rough corridor length calculates as follows: 18 mm minus 5 mm (minimum reading area height) = a 13 mm corridor length value. Note: Your calculated corridor length value may not always be obtainable in a specific progressive design. In this example, if the design you select only provides a choice between a 10 mm or 12 mm corridor, the final value chosen can depend upon additional considerations such as:
Total Frame Height and Contour: Frame style, size and shape may dictate an adjustment to your target corridor length to ensure the full reading area is not truncated by the contour of the frame’s lower rim. Pupillary distance also places a role here, with narrower PDs more sensitive to the upward slope of the frame’s nasal eyewire.
Back Vertex Distance (BVD): Closer BVDs require shorter corridors to compensate for the reduced drop of the eye’s declination intercept with the lens surface. And vice versa for longer vertex distances, which may need longer corridors.
Pantoscopic Tilt Angle: Greater pantoscopic tilt angles require shorter corridors, and lesser pantoscopic tilt angles require longer corridors. (Rule of thumb: Every 1 mm increase in corridor length will require approximately a 2-degree increase in eye declination.)
Prescription considerations can also influence your selection of corridor length:
Total Add Power: Higher add powers greater than 2.50D have smaller reading areas and higher levels of surface astigmatism (Minkwitz again). Therefore, a too short corridor (11 mm or less) may deliver compromised optics because of severe surface astigmatism.
Rx Power Change: The power change seen in a new Rx should be considered for its impact on distance vision clarity and reading declination. The direction of Rx change—more plus or less plus— is important to consider, regardless of the nature of the ametropia.
Ametropic Error: Spectacle magnification and prism may impact your corridor choice. In general, try to favor shorter corridors. The choice of a shorter corridor will assist in improving reading utility and comfort.
Lens Design Priority: The basic design priority of the lens, i.e., distance, intermediate or reading, can impact your corridor length calculation. For example, a client with a +2.00D add power may state a preference for clear edge-to-edge distance vision. Choosing a design with this priority in a frame requiring a short corridor illustrates the dilemma of optimizing a progressive to a patient’s wishes and their chosen frame style.
Non-Linear Progressive Power Gradient: Traditional progressives have featured a linear slope of increasing power. Newer free form designs utilize asymmetric slope gradients optimized for computers and users of mobile devices or for optimal driving.
VARIABLE VERSUS FIXED CORRIDOR DESIGN
Understanding when to use a variable versus a fixed corridor design is a powerful and useful tool. In the recent past, variable designs were used to prioritize the intermediate area, while fixed designs were used for prioritizing the reading area. We are talking about digital free form lens corridors, which are not to be confused with traditional molded progressives often associated with the term fixed.
Variable Corridor Length Designs: Newer variable corridor length designs optimize the corridor length to better balance reading utility and minimize swim.
Fixed Corridor Designs: Fixed designs allow the ECP to specify the vertical dimension of the reading zone to accommodate the degree of eye declination required to reach the desired add power. Fixed designs are used when prioritizing the size of the reading zone and/or the amount of eye declination required to reach the target add power. Fixed designs excel when fitting a mature add bifocal wearer greater than 2.25D add with their first progressive lens. Fitting pearl: Bifocal wearers, fitted with segments set 8 mm to 9 mm below the pupil, are well suited to using a 10 mm to 12 mm corridor referenced to a 95 to100 percent target add value. (You’re not still fitting bifocal segments using people’s lower lids without noting how far below the segment their pupils lie, are you?)
Understanding the Effects of Gaze Angles and Posture: Research to assess the normal resting and reading positions of the human eye has been extensively carried out by many lens companies, with the primary gaze angle of the eye looking straight referenced to the facial plane, defined as the line that connects the brow, upper and lower orbital bones and the jaw. The facial plane is perpendicular to the floor for a typical distance gaze, providing a distance gaze angle of zero degrees. However, depending on the frame fit, the lenses’ pantoscopic tilt results in a different angular value. Careful attention must be paid to both patient’s posture and how the fitter’s technique may affect the measured value (more on this in the section “The Problem with Posture”). And while the actual progressive transition begins at the fitting point, the initial power gradient here generally does not exceed 0.25D for the first 3 to 4 mm below the FP. This helps ensure wearer comfort and acuity within the common range of head/posture-influenced facial plane angles.
Eye declination for comfortable reading ranges from 26 to 28 degrees. But the actual near gaze angle is influenced by the wearer’s actual fitting parameters and corridor length as well as accommodation/convergence demand, posture, reading height preference, occupation, ocular motility (eye movement) restrictions or simple wearer habit. Therefore, the eyecare professional must be observant in determining a person’s actual near gaze angle as they work or read.
Then Came Smartphones: Today, progressive lens functionality issues arise from mobile phone usage. Our handheld devices are viewed closer than a book or other reading material, and our eyes are lower in the lens. Our head is down, and we use more of the lens. People older than 55 represent the fastest-growing segment of smartphone users, making this a key consideration when choosing a corridor length. Presbyopes need easy access to the reading area of the lens, but they also need a near zone area large enough to accommodate dynamic eye movements while viewing their smartphone screen.1 Today, issues arising from cell phone usage have required revising normal eye depression angles from 26 to 28 degrees to a less demanding 22 to 25 degrees.2
Wearer Preference for Shorter Corridor: We know today that depending on the interplay between the accommodative reserve and eye fatigue, wearers can momentarily tap into their accommodative reserve to achieve optimal focus while their eyes are still within the progressive corridor. This indicates the wearer’s preference for more modest eye depression angles.
The Problem with Posture: Given the above, it should be clear that one of the key elements of corridor selection is the need to assess a patient’s normal head and neck posture. From the moment you greet a client, try to ascertain if their natural posture is normal or compensatory, using the following guidelines. Normal postural habit means the wearer exhibits normal head posture when using eyeglasses. In contrast, some progressive wearers show compensatory postural habits when their new glasses differ from the previous pair in terms of fit, prescription or design change, or due to frequent postural adaptations to see a computer, tablet or smartphone screen. For example, a new Rx could reveal a change that effectively adds more plus power. This wearer may exhibit an upward head tilt, developed over time, to compensate and adapt their present weaker Rx for better reading, intermediate or distance clarity.
TIP: Knowing when to ask patients to adapt their postural habits to use their glasses effectively is just as important as knowing when not to. Time and experience are your friends here, and ECPs should avoid creating strict rules based on a few exceptional experiences. Patients should not be made to endure uncomfortable vision for some arbitrary timeframe because we assume they need to adapt. Whether the patient is having difficulty adjusting to a new prescription or this is their first progressive, they should not be sent on their way to “get used to” their new glasses without a thorough verification that the lenses are made and fit correctly.
A NEW BENCHMARK FOR OPTIMAL CORRIDOR LENGTH
Progressive lens design suffers from oblique astigmatism, which interacts optically with surface astigmatism. Molded front progressive designs favored a longer corridor to reduce unwanted surface astigmatism, particularly near the progressive umbilic, in stronger add powers. Unfortunately, accessing the full add power with the lowered reading point in these designs requires an uncomfortable eye rotation angle. Some dispensers who have shied away from short corridors should understand that free form design optimization minimizes surface astigmatism and makes short free form designs with shorter corridors much more functional with the added benefit of comfortable access. With free form fully optimized designs, the lens is personalized to accommodate the position of wear frame fit, minimizing aberrations. In addition, free form achieves an ideal balance between distance, intermediate and reading for the selected corridor length.
USING ADVANCED VARIABLE CORRIDOR FREE FORM DESIGNS
If you are ever intimidated or overwhelmed by the idea of juggling all the above factors in order to arrive at an optimal corridor length, then you can always consider selecting one of the advanced premium class fully optimized designs. These designs automatically consider all variables to strike an ideal balance between distance, intermediate and reading in selecting the final corridor length. You can maximize the customization by uploading the actual frame tracing and all the known position of wear variables. These highly customized designs may also feature the ability for dispensers to tweak the final reading height and corridor length by choosing from one of a variety of design priorities, including balanced, distance, intermediate or near.
Unleash the Power of the Corridor: A significant benefit of free form progressive technology is the freedom and flexibility granted manufacturers to create a plethora of new varied and tailored designs from which the skilled optician can choose based on frame metrics, biometrics and fit parameters. From balanced designs to those optimized for phone and tablet use to lenses with outstanding driving utility and comfort, the overall balance of a progressive design can be tailored specifically for the intended use. Even a family of designs can be created that are well suited to wearers who are sensitive to the swim sensation or those who suffer from vertigo. (This symptom previously precluded or discouraged this group from wearing progressives.) Today is a great day to be a progressive wearer and an optician!



