THE 'A-B-Cs' OF UV AND SUNWEAR - PART 1
By Andrew S. Bruce, LDO, ABOM, NCLEC
Release Date: October, 2018
Expiration Date: September 4, 2021
Learning Objectives:
Upon completion of this program, the participant should be able to:
- Be aware of the harmful effects of ultraviolet rays (UVR) on the eyes.
- Have knowledge of the science behind "light," ultraviolet radiation and the long-term effects of inadequate protection from UV.
- Be empowered with the knowledge to educate and inform your patients about the importance of protecting their eyes from harmful UVR to ensure their long-term eye health.
Faculty/Editorial Board:
Andrew S. Bruce, LDO, ABOM, NCLEC
Credit Statement:
This course is approved for one (1) hour of CE credit by the American Board of Opticianry (ABO). General Knowledge Course SWJHI550
Depending on your geographic location, enjoying outdoor activities can be somewhat limited to the time of year when the sunny weather returns to replace the seemingly endless months of rain. However, although we may be psychologically ready to see the more frequent blue skies, are we fully prepared? As a parent, when my son was little, my wife and I would always make sure he was smothered in sunscreen before we began our outdoor adventures. Myself, now paying for being a foolish fair-skinned redheaded "sun worshiper" in my teenage years, I would apply so much sunscreen that the only distinction between a clown and me was a bright red nose! As an eyecare professional, I was fortunate also to be aware of the importance of protecting my family's eyes from the sun's harmful ultraviolet radiation (UVR). However, current society does not have that awareness.
AN INFORMED AND EDUCATED SOCIETY
Dermatologists have done an admirable job of alerting the public to the risks of UVR exposure, and to a great extent, the public takes their advice seriously, using protective clothing and topical sunblock almost routinely—especially on young children who are most at risk. The eye and skin share much in common as both the eye and ocular adnexa may suffer from the same potential for damage from UVR exposure as the skin. The eye may be at even greater risk, since unlike the skin, the eye does not develop a tolerance to UVR, but becomes increasingly more sensitive with repeated exposure.
Unlike dermatology, that has implemented a highly successful public health movement to protect the skin from the adverse effects of UVR exposure, ECPs have sadly been less successful. Currently, there are no available topical sunblock preparations that can be safely and effectively applied in and around the eyes. Children are the most susceptible to UVR related eye diseases in later life and represent the smallest segment of the population wearing spectacles that can be made to provide excellent protection against UVR.
According to an AOA study, only 40 percent of Americans cite protection from sun damage as their main reason for wearing sunglasses. Also, only 28 percent say UV protection is critical when purchasing sunglasses.
In 1990, Australians implemented an aggressive campaign to increase awareness of the long-term health risks connected to UVR exposure: "Slip, Slop, Slap"—Slip on a shirt, Slop on sunblock, Slap on a hat. Due to their efforts, many Australian schools will not permit children to play outdoors in the summer months without a hat, sunblock and in some cases, sunglasses. The slogan has since been expanded to read: "Slip, Slop, Slap and Wrap!"
As eyecare professionals, it is our responsibility to educate and inform our patients about the eye health risks associated with unprotected sun exposure.
THE ELECTROMAGNETIC SPECTRUM
Let's talk about the science and physics of light for a few minutes. In the 19th century, James Maxwell determined that light is electromagnetic (EM) in nature and differed from other forms of EM radiation by wavelength only. What does that mean? Without getting too wrapped up in physics, it basically tells us that wavelength determines both the nature and effect of EM radiation.
The unit used for wavelength measurement is the nanometer (nm), 1 nm is equal to 1/1,000,000,000 (billionth) of a meter. The EM spectrum incorporates different forms of radiation ranging from "gamma rays" to "radio waves."
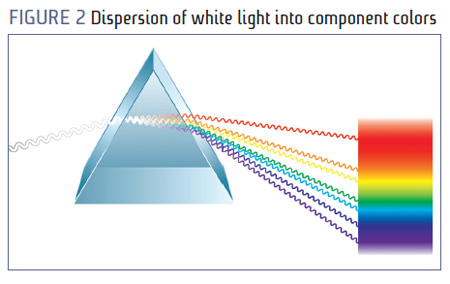
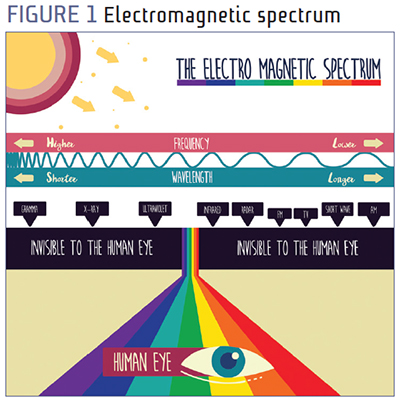 The main source of light on Earth is obviously the sun. The speed of light in a vacuum is 186,000 miles/sec (regardless of wavelength), but when passing through a medium of higher refractive index, it slows down. The degree of slowing is determined by both the wavelength of the particular component and the refractive index of the medium. Longer wavelengths are slowed less than shorter wavelengths, and a medium with a high refractive index has a greater slowing effect than a low refractive index. This slowing was described by Newton in the late 1600s as dispersion. Dispersion is defined as "the breaking up of white light into its component, or spectral colors."
The main source of light on Earth is obviously the sun. The speed of light in a vacuum is 186,000 miles/sec (regardless of wavelength), but when passing through a medium of higher refractive index, it slows down. The degree of slowing is determined by both the wavelength of the particular component and the refractive index of the medium. Longer wavelengths are slowed less than shorter wavelengths, and a medium with a high refractive index has a greater slowing effect than a low refractive index. This slowing was described by Newton in the late 1600s as dispersion. Dispersion is defined as "the breaking up of white light into its component, or spectral colors."
Example: Why does the sky appear blue? Gases and moisture in Earth's atmosphere cause dispersion of the sun's rays. Blue light, having a relatively short wavelength, is dispersed, resulting in a blue sky—commonly referred to as Rayleigh Scatter.
A material's dispersive properties are inversely related to its Abbe value as shown in the following equation (Dispersive Value = 1/ Abbe value).
Materials with low Abbe values exhibit high dispersive properties. Polycarbonate and all high index materials have a relatively low Abbe value, resulting in highter levels of chromatic aberration; some patients are hypersensitive to this and cannot tolerate polycarbonate lenses.
Chromatic aberration is a form of optical dis-tortion exacerbated by high dispersive values and results in color fringes around the images seen in the lens periphery, which can adversely affect the patient's acuity.
It causes the image formed on the principal axis by the red component of white light to be brought to a focus at a different distance from the lens than the blue component, after passing through the optical system.
In addition to wavelength's role in dispersion, wavelength also determines the frequency, intensity and energy level of EM radiation.
From the following equation, we can see how frequency is inversely related to wave-length for an EM wave: Velocity = Frequency x Wavelength
From this inverse relationship, we see that an increase in wavelength results in a decrease in frequency and vice versa. Fig. 1 also illustrates the relationship between wavelength and energy level.
EM components with shorter wavelengths propagate more energy than those with longer wavelengths.
 What significance does this have? It explains why UV-C rays, having shorter wavelengths than UV-A rays, pose a greater health risk than UV-A rays. As illustrated in Fig. 1, the EM spectrum is made up of both visible and non-visible light. "Visible white light" is only a very small portion; its approximate range is 380 nm (violet) to 700 nm (red) and is so-called because it's "that light which produces vision."
What significance does this have? It explains why UV-C rays, having shorter wavelengths than UV-A rays, pose a greater health risk than UV-A rays. As illustrated in Fig. 1, the EM spectrum is made up of both visible and non-visible light. "Visible white light" is only a very small portion; its approximate range is 380 nm (violet) to 700 nm (red) and is so-called because it's "that light which produces vision."
Our visual system works by "visible white light" reflecting off objects and the eye focusing this reflected light on the retina. The stimulated photoreceptors of the retina transport electronic signals to the brain that are then converted to visual images for interpretation. At each end of the visible spectrum are forms of light that are invisible to the human eye. These include infrared, X-rays and ultraviolet rays (UVR).
ULTRAVIOLET RADIATION
UVR is one of the main topics of discussion in this program. It can be broken down into: UV-C (100 to 280 nm), UV-B (280 to 315 nm) and UV-A (315 to 380 nm).
If we examine Earth's atmosphere, it is comprised of layers based on temperature. Their order based on their increasing distance from Earth is 1. Troposphere, 2. Stratosphere, 3. Mesosphere, 4. Thermosphere, and 5. Exosphere.
The ozone layer or shield of Earth's stratosphere is aptly named due to its high concentrations of ozone (O3) that absorbs the most harmful band of the sun's UV emissions, UV-C rays.
The ozone layer also blocks most, but not all UV-B rays. UV-B sunburn producing rays contribute to cataract development, skin cancer and eye growths such as pterygia and pingueculae.
UV-A is hardly affected by the ozone layer; overexposure causes long-term skin damage and can potentially contribute to the development of macular degeneration.
In addition to the long-term eye health risks associated with unprotected exposure to UV-A and UV-B radiation, there are also short-term risks. One such risk is photokeratitis, also known as ultraviolet keratitis and commonly referred to as "snow or light blindness."
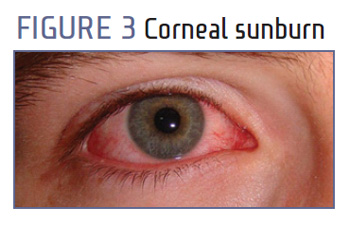 Photokeratitis (Fig. 3) is caused by overexposure of the cornea to intense UV rays; essentially, it's a sunburned cornea.
Photokeratitis (Fig. 3) is caused by overexposure of the cornea to intense UV rays; essentially, it's a sunburned cornea.
Photokeratitis results in painful temporary blindness, combined with severe photophobia and epiphora.
In 1976, atmospheric research created worldwide concern from its findings that our protective shield, the ozone layer, was showing signs of depletion. However, recent reports indicate that this depletion has, in fact, slowed down and the ozone layer is projected to recover by 2060 to 2075.
UVR levels vary throughout the day: 10 a.m. to 2 p.m. is typically the peak times. Also, UVR is higher in certain geographic areas, based on altitude and latitude.
According to World Health Organization statistics, "With every 1,000 meter increase in altitude, UV levels increase by 10 percent to 12 percent." Living at a latitude closer to the equator exposes you to higher UV levels because the sun's rays have a shorter distance to travel through the atmosphere. Therefore, less of the harmful UV radiation can be absorbed. UV levels are at their highest under cloudless skies. However, although cloud cover does provide some degree of protection, light cloud cover can actually enhance UV levels due to increased scattering. This reinforces the need for UV protective eyewear at all times. UVR is actinic radiation that is invisible yet present all the time, whether cloudy or sunny.
Unfortunately, UVR is not only ubiquitous, its impact is cumulative and irreversible. So preventative measures should be taken at an early age to protect the eyes from harmful UVR. Even though only a fraction of UV-A and UV-B rays reach the inner eye, the ocular tissues are hypersensitive to its effects.
Studies show that wide-brimmed hats and caps only block about 50 percent of UV radiation from the eyes. It is estimated that: Only 52 percent of adults who wear Rx eyeglasses also wear Rx sunwear (34 percent Rx sun-glasses and 18 percent photochromic) and only 11 percent of children who wear Rx eye-glasses wear any type of Rx sunwear (7 percent
Rx sunglasses and 4 percent photochromic). This is even more concerning because studies suggest that 80 percent of our lifetime exposure to UV rays occurs before 18 years of age. A separate report, written for Transitions Optical in 2007, indicates children's eyes are more susceptible than older eyes to potential long-term UV related damage due to the crystalline lens of a child under 10 years of age transmitting more than 75 percent of incident UV rays, compared to only 10 percent at age 30. Also, pupil diameter is larger in children compared to adults, which also allows greater UVR transmission.
The typical lifestyle of a child/teenager—extended periods in bright sunlight, combined with extended exposure to computer screens, smartphones and tablets—subjects them to not only harmful UV rays but also harmful blue light referred to as High Energy Visible light (HEV); currently, a hot topic of discussion in our profession.
Do our patients know the sources and dangers of sunlight to their eyes? According to research conducted by Wakefield Research for Transitions Optical, intended to purely investigate society's level of awareness of which types of light can cause long-term harm to the eyes, 76 percent of participants identified sunlight as a harmful source, while an additional 61 percent identified light from digital screens as a harmful source.
At first glance, these numbers are encouraging; however, the same study revealed that only 4 percent correctly identified all common sources of blue light, and only 17 percent of those surveyed recognized the sun as a source of harmful blue light, despite it emitting more than 100 times the intensity of electronic devices and screens, according to the release.
Returning to the topic of sunglasses for our younger patients, as you all know, parents are too often unwilling to invest in high-quality sunglasses for little Jimmy or Cindy. You've all heard their justifications. "They'll just break them, or lose them. I'll pick up a pair when I get the groceries next week!"
Here's where we, as eyecare professionals, have to step in and advocate for our patient by educating the parent. The estimated $1,000 the average worker spends annually at retail coffee stores clearly illustrates parents do have expendable income; if they can spend $5 to $6 every day on their "triple-shot, chocolate chai vanilla, hazelnut white mocha Frappuccino," they can afford to invest in their child's long-term eye health!
Become proficient in quoting studies. Among the two most widely cited epidemiological studies in humans are the Chesapeake Bay Waterman Study and Beaver Dam Study with results that suggest a relationship between prolonged outdoor sun exposure and the development of cortical cataracts and exudative or atrophic macular degeneration. In a follow-up study, a strong relationship was found between the time spent outdoors in the summertime during the teenage and early adult years, and the risk of early-onset macular degeneration. Results revealed that participants who were exposed to the summer sun for more than five hours a day in their younger years had a 10-year earlier onset of AMD.
Inform the parent about the differences in "Value Mart" sunglasses and premium quality sunglasses. Discuss the comparisons between important features such as the permanence of the UV protection, and the eyestrain that can be caused by looking through poor quality, cheap plastic lenses.
If the patient is ametropic, our job is much easier. Strongly emphasize the benefits of photochromic lenses as a much more convenient option for children than separate sunglasses. Children are way too active to be concerned with switching between two different pairs of glasses. However, when the patient is emmetropic, or just needs correction for near tasks, our challenge to convince the parent can be significantly greater. Regardless, we must prevail and fulfill our responsibility to our patient—the child.
The American Optometric Association's recommendations for sunglasses are: 1. Block out 99 percent of UV-A and UV-B radiation, 2. Have visible light transmission of 75 to 90 percent, 3. Lenses matched and distortion or imperfection-free, 4. Provide good color recognition and, 5. Fit close to the eye and wrap around the contour of the face to reduce rays entering from the side or bouncing off of the back of the lens. (Part 2 of this course will cover the benefits of all color tints.)
We must inform the patient/parent that not all sunglasses provide the necessary protection—a dark lens does not always indicate 100 percent UV protection.
LIGHT INTENSITY
How do we determine light or luminous intensity? The "candela" is the unit for measuring luminous intensity. The amount of light incident on a surface is measured in "lumens." One candle emits about 1 candela in all directions, which is equal to 12.6 lumens.
Examples of luminance levels:
- Indoors = 400 lumens
- Sunny day in the shade = 1,000 to 4,000 lumens (optimum)
- Sunny day in the grass = 3,500 lumens (comfort limit)
- Concrete highway = 6,000 to 8,000 lumens
- Beach or ski slopes = 10,000 to 12,000 lumens
- High altitude snowfield = Over 12,000 lumens
Computer and smartphone screen emissions are measured in "nits": 1 nit = 1 candela per square meter.
Examples of nit levels:
- Sun at noon: 1.6 billion nits
- LCD televisions: 200 to 500 nits
- Laptop screens: 200 to 300 nits
- iPhone X: 625 nits
As indicated above, the optimum luminance level is 4,000 lumens, and the comfortable limit is 3,500. Once this "comfort limit" is exceeded, the patient starts to experience ocular discomfort. Simply going from indoors to the beach can increase luminance by a factor of 30. Walking from the shady side of the street to the sunny side increases luminance by more than three times. The ocular discomfort experienced at high luminance levels is often referred to as glare.
GLARE
What exactly is glare? It is defined as a loss in visual performance or visibility, or the annoyance or discomfort produced by a luminance in the visual field greater than the luminance to which the eyes are adapted. There are two types of glare: Discomfort glare, which can also lead to eye fatigue, occurs at approximately 3,000 lumens and can escalate to disabling glare. Our natural ocular response is a slight squint. It can occur on an overcast or sunny day. The second type of glare is disabling glare; we use the acronym, BCD, a measurement of the borderline between comfort and discomfort and is measured in candelas per square meter (cd/m2). When light reaches the intensity of approximately 10,000 lumens, it has specific effects on the visual system and results in disabling or veiling glare that reduces contrast and impairs visual acuity. (Contrast is reduced due to the retinal image being scattered in the retina.)
There are also two types of disabling glare: Direct disabling glare—glare created directly from a light source to the eye, i.e., a bright sunny day and reflected disabling glare—light reflected off of horizontal surfaces, a car bumper, wind-shield, wet road or water surface. Both types of glare can overwhelm the eye with a blinding light that masks or veils the scene. When vision is impaired by glare, driving, boating and skiing and other activities can become dangerous.
 Two or more glare-producing sources are additive. The retina must re-adapt to resume vision after bleaching out of the cones by disabling glare after the bright source is removed from the field of vision. Glare, in general, becomes more problematic with increasing age, typically due to the cloudy ocular media associated with cataract development and maturation increasing lenticular light scatter. Exposure of the eye to bright light produces both a temporary and cumulative effect on the subsequent ability to adjust to varying light conditions—a process we call dark adaptation.
Two or more glare-producing sources are additive. The retina must re-adapt to resume vision after bleaching out of the cones by disabling glare after the bright source is removed from the field of vision. Glare, in general, becomes more problematic with increasing age, typically due to the cloudy ocular media associated with cataract development and maturation increasing lenticular light scatter. Exposure of the eye to bright light produces both a temporary and cumulative effect on the subsequent ability to adjust to varying light conditions—a process we call dark adaptation.
Research indicates spending just two to three hours in bright sunlight can hamper the eyes' ability to adapt quickly to nighttime or indoor light levels. This can make night driving more hazardous.
An interesting anecdote to accompany the topic of dark adaptation relates to the actual reason pirates wore an eye patch over one eye. The likelihood that it had nothing to do with a missing eye and more to do with retaining their dark adaptation in the covered eye is more realistic. This enabled them to switch the patch from the covered to the non-covered eye when going below deck, to immediately be dark adapted in the previously covered eye and see to fight when boarding and plundering another vessel.
Accumulative exposure creates long-term dark adaptation difficulties "due to the sun's sustained bleaching of the photochemical rhodopsin in the rods of the retina."
CONCLUSION
This concludes part 1 of this course. As eyecare professionals, we have a major responsibility to make sure both our patients and the parents of our younger patients are well informed and educated about the harmful effects of the sun's UV rays on the eyes. The accumulative and irreversible long-term damage potential makes the need to begin wearing UV protective eyewear at a young age extremely important. Tune in next time for the exciting sequel, part 2, which will expand upon this foundation to discuss different types of sunglass lenses, together with the pros and cons for each.



