Soft Contacts - History and Fitting Guide
By Sam Winnegrad, ABOC, NCLE-AC
Release Date: November 23, 2022
Expiration Date: November 23, 2024
Course Objectives:
Upon completion of this course participants will:
- Have a solid understanding of the history of soft contact lens development
- Understand basic anterior eye anatomy and how various conditions are related to soft contact lens use
- Have a basic understanding and working knowledge of soft lens material qualities and parameters
- Understand the importance of proper soft contact lens fitting and follow-up
Faculty/Editorial Board
 Sam Winnegrad is the Optical Director for University Eye Specialists, east Tennessee's premier ophthalmology practice. He has instructed anatomy and physiology of the eye as well as other various ophthalmic courses for Roane State Community College in Harriman, Tennessee. He has also taught for Highline College's online optician program out of Des Moines, Washington. Sam is a technical speaker for the American Board of Opticianry and National Contact Lens Examiners. Sam holds his master's degree in business administration as well as a bachelors in science - but above all treasures his license to practice opticianry.
Sam Winnegrad is the Optical Director for University Eye Specialists, east Tennessee's premier ophthalmology practice. He has instructed anatomy and physiology of the eye as well as other various ophthalmic courses for Roane State Community College in Harriman, Tennessee. He has also taught for Highline College's online optician program out of Des Moines, Washington. Sam is a technical speaker for the American Board of Opticianry and National Contact Lens Examiners. Sam holds his master's degree in business administration as well as a bachelors in science - but above all treasures his license to practice opticianry.
Credit Statement
This course is approved for one (1) hour of CE credit by the National Contact Lens Examiners - NCLE, Ophthalmic Level 2. Course # CTWJHI102-2
 We are at a point in history where medical science has
engineered and paved the way for us to be able to offer
patients the option to have their visual maladies remedied
with soft contact lenses, which only in recent years have
been available to the public. It is almost overwhelming to
contemplate the totality of human history and then to
reduce it down to the last 40 years or so of soft contact
lens use. We will first navigate through a condensed
history of soft contact lens developments. Then we will
review some of the anatomical conditions related to soft
contact lens use with potential contraindications and risks of use. Finally, we will pilot through the heart of the
course—a soft contact lens overview, where we learn how
to work with soft lenses in a practical application.
We are at a point in history where medical science has
engineered and paved the way for us to be able to offer
patients the option to have their visual maladies remedied
with soft contact lenses, which only in recent years have
been available to the public. It is almost overwhelming to
contemplate the totality of human history and then to
reduce it down to the last 40 years or so of soft contact
lens use. We will first navigate through a condensed
history of soft contact lens developments. Then we will
review some of the anatomical conditions related to soft
contact lens use with potential contraindications and risks of use. Finally, we will pilot through the heart of the
course—a soft contact lens overview, where we learn how
to work with soft lenses in a practical application.
SOFT CONTACT LENS HISTORY
Otto Wichterle, PhD, along with his wife, Linda Wichterle, MD, are largely credited with the invention of the soft HEMA lens. Wichterle and his wife worked on the first soft lens patent in the 1950s and even developed the spin casting method. Otto Wichterle was granted a patent in 1961.
This was a major step forward in bringing soft lenses to market. It was not until soft contact lenses were brought to the United States from Europe that their use began to be widely accepted in the optometric community. Other developers who were innately involved in the genesis of soft contact lens use in the U.S. were Robert Morrison, OD; Allan Isen, OD; Martin Pollak and Jerome Feldman. There is some mystique surrounding the exact chronological sequence of development and use; however, it should be noted that all the aforementioned gentlemen were integral in the development and promulgation of early HEMA lens use in the U.S.
Pollak along with the National Patent Development Corporation at first tried to entice many of the larger existing contact lens companies to purchase the patent, but they were too "myopic" to realize the impact that HEMA would have on the contact lens market. It was Bausch & Lomb who eventually bought the patent in 1966. Oddly enough, at that time, B&L was not even yet in the contact lens business. This was a game-changing decision for the company that would prove to alter the ophthalmic world. In 1968, before Bausch and Lomb was able to release contact lenses to market, the Food and Drug Administration classified these lenses as a drug. It was not until 1971 that B&L was able to hurdle the bureaucracy and gain the clearance to begin marketing its soft lenses for sale. In 1974, the brand Hydrocurve was the second firm given an FDA approval.
In the 1980s, soft contact lenses for astigmatism first became available, as well as soft lenses with a silicone component. Notable early silicone-based lenses were Silsoft designed by Ron Seger, OD, and the Dow Corning lens which was also acquired by Bausch & Lomb in 1985. Silicone dramatically increased oxygen permeability and transmission, but with the introduction of silicone into contact lens materials, we also saw an increase in lens deposition. Through the years companies have been able to minimize this foreign body attraction through various silicone compounds and lens treatments.
In the 1990s, disposable contact lenses began to gain prominence and still to this day remain the modality of choice for most providers. With the decreased wear schedule timing, manufacturers were able to present lenses that had higher silicone content, aiding in breathability and comfort, while relying on patients to heed their doctor's prescribed regimen to minimize surface malfeasants. Then in 1994, the daily disposable modality was released to the market. These lenses, as the name declares, are replaced every day. To this day, the daily disposable is touted as the "healthiest option" as the lens is not subjected to increased wear time, improper cleaning methodologies and long-term environment based molecular buildup.
Silicone hydrogel as a material was the next largest breakthrough in soft contact lens technology. Two noteworthy lenses were introduced in 1999, namely the Purevision by Bausch & Lomb and the Focus Night & Day by Ciba Vision. The hydrogel material is mainly beneficial in that it permits for better fluid transportation and enables lenses to have adequate lens movement on the cornea. Once again, the silicone in this new material is beneficial due to the markedly increased oxygen exchange. Silicone hydrogel lenses have and continue to prove their benefit in reducing the occurrence of hypoxia (a lack of oxygen); however, they do not aid in resisting deposition and decreasing the likelihood of corneal microbe infiltration.
In recent years, soft lenses have begun to make their footprint in the keratoconus and irregular astigmatism category. Many of these lenses are a hybrid design incorporating both a hard as well as soft component. The stability of soft lenses keeps improving. This is especially true with irregular types of astigmatism where the two major meridians are not 90 degrees perpendicular to one another. Most of the soft lenses used for keratoconus have thicker centers to challenge and regulate the conically shaped corneas. Wavefront lens technology is also now employed to treat irregular astigmatism levels with soft lenses. These days new lens designs are released almost monthly. The expert fitter will need to stay abreast of all developments to best utilize the given technology with their patients.
ANATOMICAL CONDITIONS AND CONSIDERATIONS
There are anatomical considerations and conditions related to the use of soft contact lenses. Contact lens technicians ought to have a solid understanding of ocular anatomy and be able to identify various conditions that could negatively impact outcomes. The eyelids by themselves can present a plethora of issues to be navigated. Some common lid issues include blepharitis, an inflammation of the lids; ectropion, where the patient's lids turn out; or entropion, where the lids turn inward. One other quite common condition is a hordeolum, an infection of a Zeis gland, which are commonly referred to as a stye. The eyelids interact with the lens and thus must be healthy enough, as to not exacerbate infection or encourage discomfort.
The conjunctive is often an afterthought but is definitely one of the most crucial determinant of successful soft contact lens wear. This membrane has three distinct regions and is in direct contact with both the external environment and the contact lenses themselves. Two of the more common conjunctival ailments are giant papillary conjunctivitis and an allergic or bacterial conjunctivitis. In basic terms, conjunctivitis is an inflammation of the conjunctival membrane. GPC has been directly linked to patients who over wear or do not properly clean their lenses while bacterial conjunctivitis starts with an infection and allergic conjunctivitis is usually tied to the presence of overall seasonal allergies. The cessation of contact lens use with all the conditions is always recommended. Other conjunctival pathologies include a nevus, which is a benign tumor; a pterygium, which is a wedge-shaped growth involving the bulbar conjunctiva; and a pinguecula, which is a round yellowish mass that is generally located along the corneal-scleral limbus. It is easy to see how any one of these anomalies could preclude the use of soft lenses.
Determining the quantity and quality of the precorneal tear film is an excellent determinant of one's success with soft contact lenses. As the first refractive surface of the eye, it is entirely necessary for patients to have a healthy sustainable tear film. Have you ever wondered why your vision gets blurry after using the computer for prolonged periods of time? This is an excellent example of how instrumental the tear film is within the optical system. As we focus on the screen, our blink rate reduces, and our eyelids do not adequately spread the tear film to create a sharp refractive layer. Interestingly, the tear film also contains white blood cells in it which are supportive in fighting infection (which is of the utmost importance as contact lens use increases the risk of ocular infection).
There are three distinct layers to the tear film. The outermost layer is referred to as the lipid layer. Its primary function is to "lock in" the tear film and prevent rapid evaporation. The next layer is the aqueous layer, which comprises the brunt of the tear film. It is secreted by our lacrimal glands and is responsible for maintaining a moist environment for the anterior of the cornea and sclera. The third layer is the mucoid layer, which is closest to the cornea. Just as the name sounds like "mucous," this layer is sticky and serves to ensure that tears will adhere to the eye.
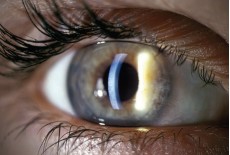 The Schirmer's test is used to determine if patients
are producing a necessary tear quantity to support
contact lens use. This is performed with filter paper
placed under the lower eyelid. The patient is given
five minutes. Less than 7 mm of wetting is contraindicative for contact lens use. The break-up-time test
is used to determine tear quality. This is performed
with fluorescein dye instilled in the eyes. Through a slit lamp, the provider will determine how long it
takes post-blinking for the tear film to start denigrating. A breakup time less than 10 seconds is a contraindication for contact lens use.
The Schirmer's test is used to determine if patients
are producing a necessary tear quantity to support
contact lens use. This is performed with filter paper
placed under the lower eyelid. The patient is given
five minutes. Less than 7 mm of wetting is contraindicative for contact lens use. The break-up-time test
is used to determine tear quality. This is performed
with fluorescein dye instilled in the eyes. Through a slit lamp, the provider will determine how long it
takes post-blinking for the tear film to start denigrating. A breakup time less than 10 seconds is a contraindication for contact lens use.
The cornea is the primary refractive medium of the eye, supplying +43.00 diopters of power. It is comprised of five distinct layers, yet is only 0.5 mm thick in its central thickest portion and thinning to 1.0 mm in the periphery. It is also in direct contact with lenses in-situ. A proper corneal evaluation is mandatory prior to any lens fitting.
There are many conditions related to the cornea that can wreak havoc on a contact lens patient. Keratitis sicca, or "dry eyes," is a very common condition where the cornea gets inflamed due to an inadequacy of the tear film to maintain the moist environment. There are drops and treatments, such as punctal plugs, that can be used to try and combat keratitis sicca to enable contact lens use. Ulcers are also all too common. This is where there is a loss of tissue in the cornea, which will appear as a pocket. Corneal ulcers are often the result of contact lens abuse, as the cornea becomes traumatized. Corneal neo-vascularization occurs when new blood vessels invade the limbus and begin to impede vision. Hypoxia stemming from either an improper tight fit or over-wearing lenses is generally the culprit as the cornea seeks other means for nutrition through the use of new vessels.
Keratoconus is a condition where the cornea becomes gradually conical in shape through a progressive thinning. Though this condition is generally treated with the use of hard scleral lenses, advancements in soft lens technology have now given rise to hybrid HEMA lenses that vault the cornea and enable visual correction depending on the severity of the case. For most patients with keratoconus, eyeglasses offer little to no benefit, so their entire world is dependent on an adequate contact lens fit.
WORKING WITH SOFT LENSES
There are so many reasons why a contact lens technician would gravitate toward the use of soft lenses. They are incredibly comfortable. This is even more true when compared to their hard lens predecessors which require a long adaptation period. Soft lenses are also much easier to fit. The base curve and diameters are limited due to their wide range of acceptance. They are also healthy when used as directed, as they offer excellent oxygen transmission with the newer materials that they are available in. These same reasons however can be the non-studious fitter's downfall. Since many lenses available offer decent comfort, it can be easy to allow an inferior fit to walk out the door. Choosing the proper modality and adequately evaluating fit, as well as following through on necessary follow-up appointments are all foundational to a successful career as a contact lens technician.
Not only are soft lenses comfortable for their obvious reason, which would be their flexibility and draping effect, but they also offer increased comfort over gas permeable and hard lenses because they generally come in larger diameters. Most hard lenses will rest on the cornea and thus will have lid interaction. That is why hard lens edge design is so crucial. Hydrophilic lenses, however, have diameters that exceed 13.8 mm and will rest under the eyelids, thus minimizing edge discomfort. This initial and continued coziness of soft lenses is also a reason why patients who once could only wear gas permeable lenses due to extensive prescriptions and high astigmatism are being moved over to soft lenses. The patient does not have to sacrifice their optics, and they can experience the increased comfort.
Children also do well in soft lenses because of the easy adaptation. It is hard enough getting a child to follow directions and maintain proper hygiene to support contact lens use, but it is even more difficult if the lenses themselves are not comfortable. It is much more difficult for the child to be motivated to properly wear and care for their lenses. Many children desire contact lenses because they are active in athletics. This can be the impetus for a contact lens examination. Hydrophilic lenses can be superior to gas permeable lenses for sports because they are less likely to become dislodged from the eye during rigorous activity, whereas hard lenses may "pop out" if a child is tackled or any other potential severe sport induced jostling.
Soft lenses can also be superior to gas permeable designs when the environment is a factor. Many factory workers or employees of dusty high-debris environments are more at risk for vocational particles to creep under hard lenses, while it is much more difficult for these particles to find their way under a soft lens, largely due to their greater diameters and draping effect over the cornea.
 On the other hand, hydrophilic lenses may be
unsuitable for some environments as they can easily
dry out and dehydrate in certain conditions. They
are also exceptionally good at absorbing gasses, so if
your patient works with noxious fumes, it may be a
strong contraindication. Furthermore, the lenses are
notorious for absorbing hairspray, makeup and
other chemicals such as the ones found in their
cologne. This is why proper training and potentially even a daily disposable modality ought to
be considered.
On the other hand, hydrophilic lenses may be
unsuitable for some environments as they can easily
dry out and dehydrate in certain conditions. They
are also exceptionally good at absorbing gasses, so if
your patient works with noxious fumes, it may be a
strong contraindication. Furthermore, the lenses are
notorious for absorbing hairspray, makeup and
other chemicals such as the ones found in their
cologne. This is why proper training and potentially even a daily disposable modality ought to
be considered.
Giant papillary conjunctivitis (GPC) is a major concern when considering soft contact lenses. Since surface deposition is common in soft lenses, GPC is more prevalent than with gas permeable patients. The palpebral conjunctiva will experience an allergic reaction to the deposits in the lens and will respond accordingly with inflammation and well, giant bumps under the lid. GPC is generally a recurring issue. There are ways to prevent it, such as using daily disposable lenses, but once a patient first is diagnosed, it will be more likely for GPC to occur again and again. Proper lens cleaning is paramount in thwarting GPC. There is a good chance that your patients with giant papillary conjunctivitis over wear or do not adequately clean their lenses.
Knowing which lens material to choose is an important part of attaining the best fit. This is where we consider the implications of water content, oxygen permeability, resistance to infiltrates and even edge design. Maybe soft contact lens fitting isn't that easy after all.
The oxygen permeability of the lenses that you select will have a dramatic effect on the overall success of your patient. Lens manufacturers express this value as Dk value. The factors that will affect a lens' Dk value are the center thickness of the design, the water content and the lens' ability to resist deposition. Obviously, a lens with a thinner center and the ability to resist deposits will enable greater oxygen transmission than a lens with a thicker design and poor deposit deflection.
Selecting a lens with a high-water content increases the flexibility of the material but is at increased risk of poor optics. Low water content lenses, almost counterintuitively, require a lower tear production as do the higher water content lenses. Do not forget to talk to your patients about the benefits of artificial tears, as lens dryness is something that most patients will encounter at some point in their use of lenses.
Edge design is an important factor in overall lens comfort. In general, thinner edges are more comfortable to the wearer. Patients may reject a lens due to the material itself, the edge design, base curve, diameter, optics, rotation, etc. As an eyecare professional, you must be diligent and employ deductive tactics to properly determine a proper solution. This is also true in determining the modality type, such as daily disposable, bi-weekly disposable, monthly and so on. The fitter must be confident knowing that their patient understands and can follow the proper regime.
 The parameters that a lens technician must be
comfortable with include base curve, diameter and power. A three-point touch is desired. This is
when the contact touches upon the center of the
cornea and the two opposing sides of the sclera.
This fit requires a proper sagittal depth which is the
vaulting of the lens over the cornea and is determined by base curve and diameter selection.
The parameters that a lens technician must be
comfortable with include base curve, diameter and power. A three-point touch is desired. This is
when the contact touches upon the center of the
cornea and the two opposing sides of the sclera.
This fit requires a proper sagittal depth which is the
vaulting of the lens over the cornea and is determined by base curve and diameter selection.
Eyecare professionals must be proficient in keratometry or some form of corneal topography to select the best base curve option. Knowing the corneal K readings will be helpful in selecting the appropriate base curve, as well is also necessary to make sure that the eyecare professional can monitor the cornea over time for any changes. The average cornea will present K readings between 42.00 and 45.00 diopters. Most soft lens manufacturers offer lenses in only a few base curves, so it is incredibly important to choose the right one. In general, it is best to start with a flatter lens and go steeper as necessary.
Measuring a patient's HVID and palpebral fissure will set the stage to determine the best diameter. A soft lens will cover the cornea and bridge the limbus, resting on the anterior sclera. If a lens is too small, it will not be as stable and may not be comfortable if the lids are interacting with it. The average visible iris diameter is 11.5 mm. We generally want to select a lens that is at least 2 mm larger than this to allow for adequate movement.
What good are the perfectly fitting lenses that you just selected if the patient cannot see out of them? There are some general rules of thumb for selecting the appropriate soft lens power. A soft contact lens power is derived from the final eyeglass refraction. While working with contact lenses, we always want to make sure that this refraction is in minus cylinder form. The next consideration is vertex compensation if the eyeglass prescription is +/- 4.00 diopters or higher. Vertex distance has a negligible effect on lower strengths. There is a multiplicity of vertex compensation charts available for our use, but the primary thing to remember is that contact lenses act more minus in situ because all lenses effectively gain plus strength as they are moved farther from the eye. For example, if a patient is refracted with the phoropter 14 mm away from their eyes at -5.50 diopters, that same patient with a -5.00 diopter contact lens resting on their cornea would yield the same visual effect.
When patients with prescribed cylindrical correction are being fit, the eyecare professional can either use the spherical equivalent of the eyeglass prescription if there is less than one diopter of cylinder, or they will need to choose the appropriate toric lens if it is 1.00 diopter or greater. To determine spherical equivalent, just add half of the cylinder to the sphere. If a toric lens is required, always select the lens power that closest matches the refraction. If the exact strength is not available, use the lower option. Allow the lens to equilibrate for a minimum of 15 minutes before checking axis alignment with a slit lamp degree scale. Equilibration is the process by which the contact lens settles in and hydrates with the patient's tears. Using the 6 o'clock marking on the equilibrated lens, the fitter can determine if the lens is stable or has rotated to the left or right. We use the acronym LARS to remind us that if it has rotated to the left, we add that amount of rotation to the original refraction, and if it has rotated to the right, we subtract the amount from the original refraction. If a slit lamp degree scale is not available, it is possible to use the rule of thumb that every hour on a clock represents approximately 30 degrees.
In evaluating a diagnostic lens for a patient, there are five areas that must be assessed. They are corneal coverage, movement, three-point touch, comfort and visual acuity. All of these five areas must have a positive evaluation for the fitting to be a success.
Using a slit lamp with a diffuse illumination, the fitter can evaluate if there is enough corneal coverage. Remember that theses lenses are supposed to center properly, vault the limbus and should rest approximately 1 mm past the limbus. This is why we select a lens that is approximately 2 mm larger than the HVID. The lens should also have adequate movement with blinking. When the lenses move, it allows for increased oxygen exchange as well as permits for debris and foreign bodies to be sluffed away into the tear stream. Most manufacturers recommend 1 mm of movement while blinking.
If a lens is properly fit, it will exhibit three-point touch. This means that the lens touches upon the center of the cornea and the two opposing sides of the sclera. There are three ways to determine if three-point touch is present; by looking at the mires with keratometry, by viewing the retinoscopic reflex through the lenses, or by simply checking visual acuity. A lens that is properly fit will also not flex during blinking, creating both distorted keratometry mires and distorted vision for the patient. If the lens is not exhibiting three-point touch, a change is needed with the sagittal depth, which is the relationship between the base curve and diameter of the lens.
Patient comfort is a large part of the successful soft contact lens fitting. A lens can be uncomfortable for many reasons including edge design, thickness, defect, diameter, solution used, etc. Sometimes a lens will become more comfortable after equilibration, and sometimes it will take longer. If comfort does not improve, it is an unsuccessful fit and you must determine the reason. Likewise, if a patient's vision is not what it should be, then it is necessary to perform spherical and then spherocylindrical over-refractions and select a more accurate dioptric power.
Follow-up visits are a necessary part of fitting soft contact lenses. Seek your patient's subjective input by asking questions revolving around lens comfort and visual acuity. Then it is necessary to perform an objective evaluation, no less invasive as the original fit. This is where we re-visit areas such as corneal coverage, movement, three-point touch, comfort and visual acuity. It is also important to review the overall condition of the lens in situ and to evaluate if there are notable surface deposits, and since contact lenses are in contact with the cornea, a full corneal evaluation is also recommended with and without fluorescein dye.
CONCLUSION
Soft lenses are such a commonality in our practices that it is easy to forget their relatively short history. As a fitter, it is important to understand some of the dangers and woes associated with hydrophilic lenses. We must then be able to take a vast amount of information into consideration for each patient that is wearing or desires to wear these lenses. The risk is to oversimplify the process since manufacturers have spoiled us with standardized base curves and other "blanket" parameters—not using due diligence to ensure the proper fit is attained and the most desirable outcome is achieved.



