BLUE LIGHT REFOCUSED
– SEPARATING SCIENCE FROM SPECULATION
By Gary Morgan, OD
Release Date: June 1, 2017
Expiration Date: July 1, 2018
Learning Objectives:
- Understand what blue light is and the role it plays in visual and non-visual function.
- Recognize the importance of light transmittance curves when evaluating blue light attenuating lens products.
- Differentiate between unsubstantiated product claims and actual science when positioning blue light attenuating lenses in the dispensary, and framing conversations about them with patients.
Description:
As the topic of blue light has come to the forefront in the ophthalmic industry, the line between science and commerce has become blurred. Science based discussion has focused on three areas, AMD, sleep disruption, and ocular discomfort.
This course will provide opticians with the ability to properly present blue light attenuating lenses based on scientific facts and statistics.
Credit Statement:
This course is approved for one (1) hour of CE credit by the American Board of Opticianry (ABO) Technical Level II, Course STWJHI662-2.
Faculty/Editorial Board:
Gary Morgan, OD has been in private practice for 25 years in Arizona, with an emphasis on the care of patients at risk of, or with AMD. An advocate for innovation, he serves in a technical advisory capacity to ophthalmic industry enterprises focusing on spectacle lenses, nutraceuticals, and telemedicine that are intent on lessening the effects of AMD and blue light.
Supported by:
This course is supported by an educational grant from VSP Optics Group.
VISUAL BEHAVIOR AND ENVIRONMENT, A PARADIGM SHIFT
In the last 10 years, two events have occurred that have altered our visual behavior and environment unlike any others in human history.
First, mobile-connected digital devices including smartphones and tablets have become the mainstay of how we receive and transmit information. Their screens are backlit by LED bulbs.
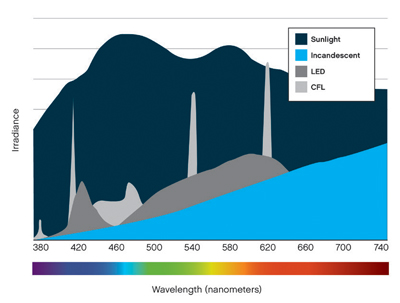
Second, by legislation, incandescent light bulbs are being replaced with more energy efficient CFL and LED bulbs. However, as with any time advances in technology are made, there may be unintended consequences. As seen in Figure 1, we have had an unprecedented increase in blue light exposure. And it is blue light that is the source of this extraordinary change in our visual behavior and environment.
SPECTACLE LENSES, MORE THAN VISION CORRECTION
Historically, correction of refractive error has been the primary purpose of spectacle lenses. Secondarily, spectacle lenses have been used for workplace safety, and sun protection, primarily blocking UV light. However, a new era is upon the optical industry; attenuating short wavelength visible light (blue light) indoors to promote eye health and safety.
The scientific literature, detailing what is known and unknown about blue light and how it affects human vision and health is evolving. This science can be complicated, however all eyecare providers should endeavor to learn the facts to properly present new blue light attenuating lenses to patients. Admirably, the optical industry has responded rapidly to introduce products to attenuate blue light, however product claims are sometimes not substantiated by the science. It is the responsibility of all eyecare providers to separate science from speculation.
2016 REPORTS CAUSE FOR CONCERN
Two reports published in 2016 by The Vision Council and by VSP Vision Care demonstrate the enormity of this problem. What is interesting about the timing of these reports is that scarcely five years ago, the subject of blue light exposure and its effects on the eye were fringe topics in eyecare. However within the last five years, the amount of blue light education presented for ophthalmology, optometry, and opticianry has increased significantly. And it is not just professional awareness that has increased. Mainstream media reports have increasingly discussed the dangers that blue light exposure may pose.
Highlights of The Vision Council report are that 90 percent of Americans use digital devices for two or more hours per day, 60 percent use them for five or more hours, and 65 percent experience symptoms of digital eye strain. 77 percent of individuals who suffer from digital eye strain use two or more devices simultaneously, yet 90 percent don’t discuss visual symptoms from device usage with their eyecare provider. About one third of respondents were unaware of computer-specific eyewear.
VSP’s report states that by the time the average American child reaches age 17, they will have spent over a third of their lives looking at digital devices. Parents are concerned about their children’s excessive screen time, with 44 percent stating they feel their kids are addicted to digital devices. Yet the majority, while perhaps having a parental inkling that something is wrong, are unable to specifically identify a problem with device usage. 58 percent of parents had little to no awareness that high-energy blue light is emitted from digital devices, and only 10 percent had taken steps to safeguard their families from blue light.
THE ELECTROMAGNETIC SPECTRUM AND WAVELENGTH OF LIGHT
As inhabitants of the earth, we are surrounded by waves, some damaging, some benign. Wavelength is the key to understanding which waves cause harm. Shorter wavelengths have higher energy with greater potential to cause damage, while longer wavelengths are relatively harmless. All waves are part of the electromagnetic spectrum. Visible light wavelengths, 400 nm to 750 nm used for human vision, make up a fraction of the total electromagnetic spectrum. Adjacent to the shortest visible light waves are UV wavelengths ranging from 100-400 nm.
Blue light is defined as wavelengths from 400-500 nm. Note that this is adjacent to UV light and has the shortest wavelength (thus the highest energy) of visible light. Blue light is able to penetrate the cornea and lens and is incident on the retina. Science links cumulative lifetime blue light exposure from sunlight to the development of age-related macular degeneration (AMD), the leading cause of blindness for those over age 55 in developed countries.
HOW THE EYE PROCESSES LIGHT: VISUAL AND NON-VISUAL FUNCTION
The human eye contains three types of photoreceptors. Cones and rods are responsible for visual function. Cones are located in the macula, are active in bright to dim environments, provide color vision, and are responsible for detailed visual acuity. Rods are located outside the macula, are active in dim to dark environments, are not capable of color vision, and do not provide detailed visual acuity. Intrinsically photosensitive retinal ganglion cells (ipRGCs) are responsible for nonvisual function. They are located throughout the retina and contain the photopigment melanopsin, a key mediator of non-image forming neurologic pathways.
HOW VISIBLE LIGHT BEHAVES IN THE EYE
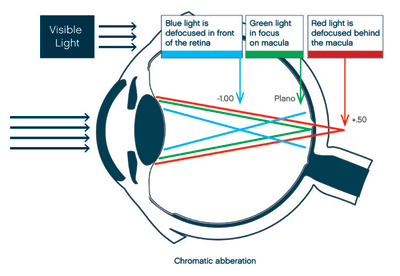
Blue light is detrimental to vision in that shorter wavelengths are out of focus, and the retina lacks processing power for it. The macula contains predominantly long wavelength red cones, followed by medium wavelength green cones, with only 2 percent of cones being short wavelength blue. In Figure 2, we can see that in the refractively corrected eye, green light is in focus on the macula. Longer wavelength red light is mildly hyperopically defocused, by approximately +0.50D. Shorter wavelength blue light is significantly myopically defocused, by approximately -1.00D. This creates a violet-blue blur circle, or haze around the in focus green component of light. This phenomenon is known as chromatic aberration and significantly affects visual quality. Blue light diminishes visual quality in that its short, out of focus wavelengths reduce contrast. It is well known that brown sun lenses enhance contrast. This is due to the fact that brown tints limit blue light. Glare, defined as exposure to a light source exceeding our retinal adapted state, also diminishes visual quality. Glare is worsened by blue light as its short wavelengths are scattered the most intraocularly. Blue light sources such as electronic screens or the sun can worsen glare, causing discomfort or disability depending on brightness.
DIGITAL EYE STRAIN
When viewing electronic devices, myopically defocused blue light results in what is now termed digital eye strain. The Vision Council defines digital eye strain as “the physical eye discomfort felt by many individuals after two or more hours in front of a digital screen”. In a 2014 survey conducted by VSP, eyecare providers reported a 50 percent increase in patient complaints of digital eye strain and effects of blue light exposure. Also stated was a 38 percent increase in these same complaints from children. Without intervention, reports containing statistics such as these will likely increase.
The symptoms of digital eye strain can be broken down into three causes: proximity of the light source (digital device) to the eye, intensity of light from the source, and frequency and duration of exposure. In considering ways to alleviate symptoms, keeping these causes in mind can guide treatment recommendations.
Proximity. We tend to hold digital device screens closer to our eyes. This increases demands placed on our accommodation and vergence systems.
In a 2011 study published in Optometry and Vision Science, it was demonstrated that mean working distance is decreased when viewing digital devices. In comparison to the 16” distance that a typical adult holds hard copy text, when using a smartphone, working distances decreased. Their findings showed that when viewing a text message, working distance decreased to 14.25 inches, and when viewing websites, to 12.68 inches. They state that these closer working distances will place increased demands on accommodation and vergence, especially with extended viewing time. Consequently, symptoms of visual discomfort may be exacerbated when compared to longer viewing distances used when reading hard copy material. They conclude that practitioners need to consider closer distances adopted while viewing material on smartphones when examining patients, and prescribe refractive corrections based on closer working distances. In other words, standard age appropriate add powers need to be increased to adjust for closer working distances, especially when treating patients presenting with asthenopia associated with digital device usage.
Intensity. The Intensity of light from digital devices is dependent on the distance the device is held from the eyes.
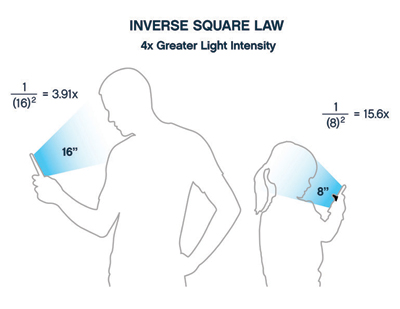
If you are familiar with lighting and photography, you know that the Inverse Square Law states that the intensity of a light source is equal to 1 over the distance squared (Figure 3). What this means concerning light exposure is that a child holding an iPhone or iPad at 8 inches is getting approximately 4 times the light, including blue light, as an adult holding the same device at 16 inches. And as discussed above, adults are holding smartphones closer for viewing text messages and websites, increasing the light intensity their eyes receive. This added light intensity can affect the feeling of fatigue we experience from using digital screens.
Frequency and Duration of Exposure. The number of times during the day that we look at digital screens and the amount of time spent looking during each episode affects symptoms of digital eye strain.
Evidence of increasing frequency and duration of exposure to hand held digital devices is all around us; just observe tables of people in restaurants all looking at their smartphones. A recent report showed that in 2014, the minutes per day spent looking at mobile-connected digital devices surpassed the number of minutes spent looking at a TV screen.
BLUE LIGHT AND NON-VISUAL FUNCTION
With the discovery of intrinsically photosensitive retinal ganglion cells (ipRGCs) in 2002, it has been shown that light travels to all areas of the brain, not just the visual cortex. In terms of blue light, several studies point to wavelengths between 459-484 nm as having the most effect on ipRGC function. Although research on these cells and their function is still in its infancy, it is understood that ipRGCs exert some degree of control over circadian, pupillary light reflex, and neurobehavioral response.
ipRGCs contain the photopigment melanopsin, which absorbs light and is vital to their function. Melanopsin is the key component of non-image forming pathways, which on a species level are more primitive than rod and cone visual systems. This allows for non-visual sensing of light needed for survival. In humans, ipRGCs are the first photoresponsive cells of the retina to develop, capable of detecting light embryonically. They are also some of the last retinal neurons to die, with photoreceptors (rods and cones) being more susceptible to degenerations and disease such as glaucoma, diabetes, and AMD.
CIRCADIAN RHYTHM
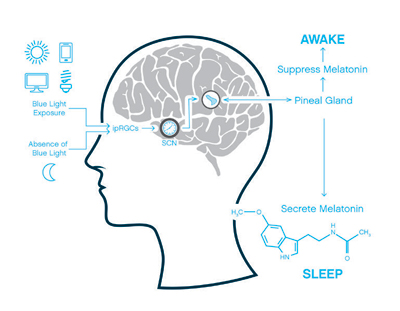
Circadian rhythm can be thought of as regulating our sleep – wake cycle. Historically, human exposure to blue light at night was relatively low. Daytime exposure to blue light, would trigger our internal clock to suppress melatonin secretion, keeping us alert and awake. As evening would fall, lack of blue light would allow for secretion of melatonin with subsequent onset of sleep (Figure 4). However with advancements in technology, our evening exposure to blue light is at levels never before experienced by mankind. Electronic screens on our smartphones, tablets, and computers, as well as LED and CFL light bulbs, all emit light 459-484 nm blue light affecting ipRGC function.
Studies show we are all sleeping less than previous generations, and our technology boom of the last 10 years is feeding into this.
PUPILLARY LIGHT RESPONSE
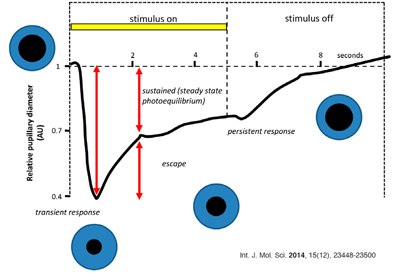
When exposed to a bright light, the pupil rapidly constircts (Figure 5).
This fast initial constriction is largely mediated through the visual pathway, and is predominantly driven by cone photoreceptors.
After this initial fast phase of constriction, the samller pupil size is sustained by a combination of the light adapted cones, along with a steady-state ipRGC response. This response is maintined until the light source is removed, and the pupil dilates back to its normal size.
NEUROBEHAVIORAL ASPECTS OF BLUE LIGHT
Research continues to evolve on ipRGC function showing blue light’s effect on neurobehavioral aspects of conditions such as mood, depression, addictive behavior, and pain avoidance. For instance, seasonal affective disorder (SAD) has been linked to human mutations of melanopsin contained within ipRGCs. SAD is associated with mood and physiological changes evident in winter months for some individuals. These changes are due to shorter daylight hours, thus less exposure to natural blue light. Therapies using long blue wavelength light (460-500 nm) have been successful in helping to relieve symptoms.
BLUE LIGHT ATTENUATING LENSES, SPECTRAL TRANSMITTANCE CURVES
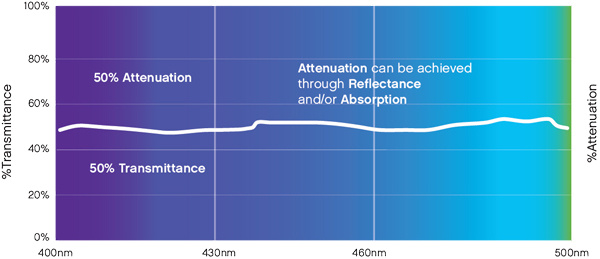
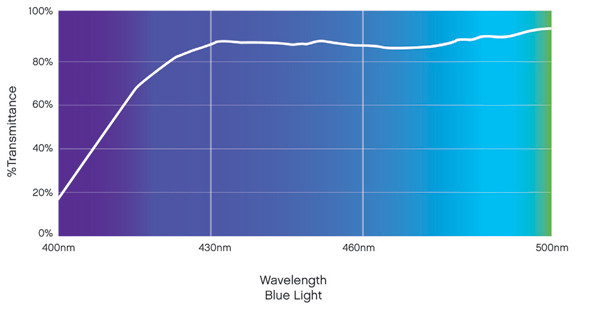
The first thing one must look to when deciding the merits of a blue light-attenuating lens is its spectral transmittance curve (Figure 6). This is akin to knowing components and side effects of a drug, we must know what we are prescribing. An important point to remember is that lenses do not block a fixed percentage of blue light. The percentage of light blocked is wavelength specific. So while a specific lens may attenuate 80 percent of blue light at 405 nm, that same lens may also attenuate 10 percent of light at 440 nm. It would be disingenuous to claim that this lens blocks, say, 40 percent of blue light; clearly it does not (Figure 7).
TYPES OF BLUE LIGHTATTENUATING LENSES
While blue light-attenuating lenses represent a new category, some components of them have been around for many years. Lets take a look at the avaialble catagories and how each one works.
Infused lens materials have pigments or dyes added to the lens monomer absorb blue light. They provide attenuation along entire blue light range, with their strongest effects at the shortest wavelengths. Some have a characteristic yellow coloration. New generations of infused lenses are nearly clear in appearance. Masking dyes are used to offset yellow coloration. However, this may result in dips in transmittance from 480-550 nm, which may affect both visual performance as well as ipRGC function. Whether this effect on visual and nonvisual function of retinal photoreceptors is significant is currently unknown.
Lens coatings reflect blue light by inducing selectively disruptive light interference. This induces a characteristic purple to bluish color in these lenses, and they have a modest effect on the shortest blue light wavelengths.
Multifunctional lens coatings both absorb and reflect blue light through the use of both multi-layer thin film coatings combined with rare earth compounds and minerals. They have a significant effect on shortest blue light wavelengths associated with visual strain and fatigue.
The cosmetic appearance of theses lenses is moderated due to combination of absorptive and reflective characteristics, resulting in a mild blue coloration.
Photochromic lenses provide variable blue light attenuation depending on their adaptive state. Photochromic nanoparticles “unfold” when exposed to UV, absorbing blue light, blocking UV, and appearing colorful. When the UV source is removed, the nanoparticles gradually return to their original state and appear colorless, however they retain some of their blue light absorptive properties.
With over 100 blue light attenuating lenses available, it is impossible to present all of their transmittance curves in this article. Eyecare providers should embrace the use of transmittance curves; we should know what we are prescribing. However, while some companies readily supply this information, others do not.
BLUE LIGHT AND LENS PRODUCT INFERENCES
The explosive growth of the blue lightattenuating lens market over the last five years has brought with it some product inferences. Product literature often discusses the three effects of blue light on the eye, AMD, sleep disruption, and visual strain and fatigue. To clinicians and consumers alike, this information may be misleading.
It is now believed based on peerreviewed scientific evidence that both oxidative stress and cumulative lifetime exposure to blue light contribute to the development of AMD. Blue light lens products are often marketed to digital device users, as digital device screens emit blue light. However, there are no current studies that link digital device or electronic screen usage to AMD, and there are no lens products on the market that are clinically proven to diminish the risk of developing AMD. As such, care must be taken when discussing potential protective effects with patients.
As discussed, ipRGCs are most sensitive to blue light in the 459-484 nm range. When exposed to these wavelengths after dark, melatonin secretion can be adversely affected. At this time, recommending blue light-attenuating lenses to improve sleep is not appropriate as there is no FDA approved indication for this. In fact, with current technology, lenses to improve sleep would need to be a very deep brown color, not practical for indoor, after dark use.
However, based on basic ocular anatomy and physiology, it is well known that blue light has a detrimental effect on visual function. There are blue lightattenuating lens products on the market now that diminish the effects of blue light from artificial light sources to improve visual comfort. This makes prescribing blue light-attenuating lens products clinically appropriate and is their best current application, especially for relief of digital eye strain.
CONCLUSION
The largest shift in the history of humankind on visual environment and behavior has occurred. As eyecare professionals, staying abreast of new developments in the science of blue light and products to combat its effects are vital to both the health and welfare of our patients and practices.