
Photograph By Ned Matura
By Palmer R. Cook, OD
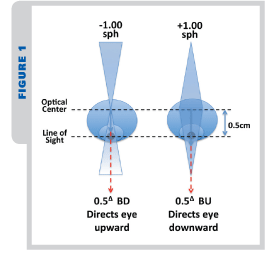
Most of our patients have only a limited ability for making a “one eye upward, the other downward” adjustment. A patient with -1.00 OD and +1.00 OS will have little difficulty looking through the optical centers of his lenses. However, if he looks 0.5 cm below the optical centers, he will have .5∆BD directing the right eye upward. Because the left eye will also be looking 0.5 cm below the OC of the left lens, the left eye will have to be directed downward by .5∆. The result: The patient faces the challenging task of making an upward movement with one eye and a downward movement with the other. Worse, as the patient raises or lowers his chin, the amount of vertical prism disparity1 will vary with every movement.
 SINGLE VISION ADAPTABILITY
SINGLE VISION ADAPTABILITY
Part of the above patient’s adaptation to new lenses will consist of finding just how much he must raise his chin to look upward, and how much he must tuck his chin down to look downward to be close enough to the OCs to see with comfort and no diplopia. Patients with single vision lenses and a vertical imbalance2 usually learn to change their head positioning so their lines-of-sight are fairly close to the level at which you have placed their Major Reference Point3.
INDIVIDUAL SENSITIVITY
Most patients can adjust to about .5 prism diopters (.5∆) of vertical imbalance. Greater amounts of vertical imbalance lead toward discomfort, blur, disorientation and diplopia. To avoid these problems, a patient faced with the need to fuse images that are vertically disparate: A. Develops a greater range of fusional ability. B. Learns to suppress one of the images, and C. Learns to move his head or eyewear so the demand for vertical fusional movement is decreased. Sometimes patients develop a combination of these adaptations.
Those who must look through a lower area in their lenses for reading or computer work and a higher area for distance seeing present us with a more complicated situation.
BIFOCALS AND MULTIFOCALS
With bifocals or multifocals, the MRPs are typically placed so that both lines-of-sight pass through the optical centers or sufficiently close to the optical centers when the patient is standing and looking at a point on the floor about 17 feet ahead. Usually these patients are comfortable for near work if the bifocal segs are placed about 4 to 6 millimeters below the centers of the pupils and with the patient’s head in its “normal” position. This allows most patients to read comfortably at about 10 millimeters below the distance MRP, or about 6 or 7 millimeters into the seg. For trifocals the reading level is placed several millimeters lower. If a vertical imbalance is present, the amount of vertical disparity is calculated at the reading level after the MRP locations are determined.
WHY ARE PALS DIFFERENT?
PALs do not have an MRP. Typically, the optical center is at the Prism Reference Point (PRP), which may fall 8 millimeters below the Distance Reference Point (DRP). The Near Reference Point (NRP) may fall as much as another 12 to 18 millimeters lower. The DRP is the height at which the major ray bundle clears the top of the corridor. This closely represents the height at which the MRP should be placed if multifocals were being used. For multifocals, the drop to the reading level would be about 10 mm for a bifocal and slightly longer for a trifocal. Another difference is that the slab-off line placement is fixed (with rare exception) at the seg line for multifocals, and the placement is arbitrary for PALs.
THE BIG QUESTION FOR DISTANCE VISION
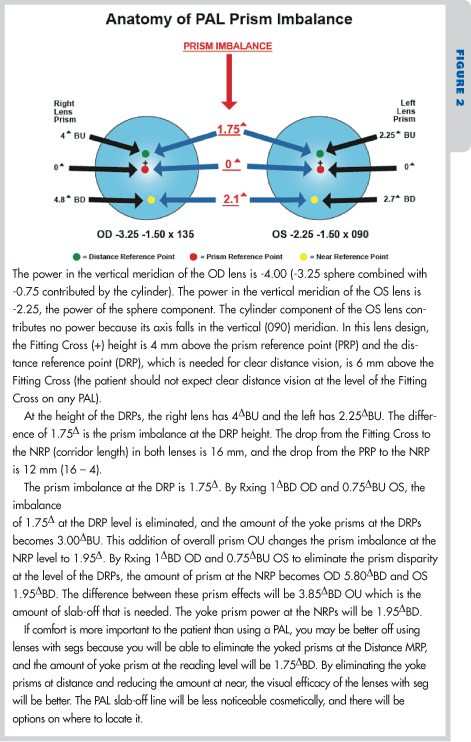
Will your patient be able to maintain clear, comfortable, binocular vision when his lines-of-sight are passing through the DRP? In the Fig. 2 example, without Rxing vertical prism he would have to fuse 1.4∆ of vertical imbalance. If he raised his head to the point at which he had a .5∆ imbalance (2.86 mm above the PRP), blur for distance seeing will occur if his major ray bundles impinge on the lens corridor. It is possible that your patient would feel his distance vision is “marginally satisfactory” or worse.
THE BIG QUESTION FOR NEAR VISION
It is unlikely that the patient in Fig. 2 will be able to maintain clear, comfortable, binocular vision at the level of the NRP (2.1∆ of vertical imbalance without vertical prism). To reduce the imbalance to an amount he can comfortably fuse, he would have to raise his lines-of-sight to a point at which the add power would be too weak for reading distance. It is probable that your patient might consider his lenses “not satisfactory” for near point tasks. If vertical prism (1∆BD OD and .5∆BU OS) were used to correct the prism imbalance at distance, the prism imbalance at near becomes 2.6∆, so a 2.6∆ slab-off will be needed.
Clinical Suggestions
and Guidelines
- Patients with small pupils may have the ability to achieve clear distance vision at a level somewhat below the distance reference points (DRPs), the points at which your lensometer must center in order to correctly measure the distance power of the lenses.
- By selecting a PAL design that has a shorter drop from the DRPs to the PRPs when a patient has differing powers in the vertical meridians of his lenses, you may make him more comfortable. This only works with small imbalances.
- By selecting a PAL design that has a shorter drop from the PRPs to the NRPs (i.e., using a shorter corridor) when a patient has differing powers in the vertical meridians of his lenses, you may make him more comfortable. This works only with small imbalances.
- Train your staff to routinely compare the powers in the vertical meridians of every prescription. Explain the use of off-axis power charts when the prescriptions have cylinder. Off-axis charts should be available from your lab or visit opticampus.com/tools/vertical.php for a vertical imbalance calculator.
- When significant imbalance is present, consider the alternatives of contact lenses instead of glasses or the use of one pair of glasses for distance and another for near—an approach that is common in Europe.
- The option of equalizing the power difference using one contact lens is an option that can work in some cases.
- Although slab-off with bifocals or multifocals usually allow the patient to have clear vision without any prism at the distance MRP height, PALs typically require the patient to have some prism at the level in the lens that gives the prescribed distance power. Using the available technology that you would prescribe for any patient needing prism is especially important. These tools are AR lenses, the lowest practical index material for the Rx and possibly a light tint or a photochromic lens with some residual tint.
- When designing a slab-off for a PAL, adjust the frame completely before taking any measurements as with any PAL, and mark a line on the lenses to represent the location you would feel appropriate for the slab-off line. Then observe the patient’s habitual head position and discuss their normal vision-related tasks. Looking through the slab-off line causes monocular diplopia and some related adaptation problems.
- If you wish to use bifocal trial lenses for demonstration purposes, ask your lab to make plano carriers with the add powers in pairs (i.e., +1.25 adds in D-28s, +1.75 with a 50 percent intermediate in trifocals and a +1.25 add in the PAL of your choice). These lenses are quick and easy if you want to introduce new or advancing presbyopes to the concept of needing differing powers for different viewing distances. They also allow you to use a plano prism to demo the actual effect of including slab-off in the new eyewear.
- Patients with undiagnosed vertical phoria/tropia problems often have a history of adaptation problems and often work their single eyewear so one lens is higher, and the other is lower to correct or partially correct their vertical muscle problems. These same patients tend to tilt their head behind the phoropter when binocular acuities are taken. The doctor’s protocol should be to observe the fit of the current eyewear and to use pinholes to center the patient for testing. Depending on the Rx, these patients tend to hit the wall when PAL or even lenses with segs are prescribed.
—PRC
See the last bullet point in the “Clinical Suggestions and Guidelines” sidebar and the comments in “The Solution” section of this article. Also, the doctors should be doing vertical vergence testing. This gives strong clues about whether slab-off should be used. The power of the add is immaterial to the amount of slab needed, and most long-term anisometropes have coped one way or another, unless the imbalance has changed dramatically and suddenly.
ORDERING
It is better not to specify the amount of slab-off. Instead, order the slab-off specifying: “Slab-off for no vertical imbalance at the height of the NRP, and add prism as needed to give no prism imbalance at the DRP.” By doing this, any error in calculating the slab-off is the responsibility of the lab, and you can use your lensometer to easily verify that the slab-off and distance prism are correct by measuring the prismatic imbalance, if any, at the height of the NRP. Some labs may only be able to provide PAL slab-off powers in quarter diopter steps, so rounding the slab-off power may limit the vertical dimension of the effective reading “sweet spot.”
Keep in mind that patients can tolerate some imbalance, and they can also self-compensate by looking a bit above or below the NRP as long as they are getting the correct dioptric power. If you elect to fit a PAL with a slab-off, ask the lab to calculate the needed amount of yoke prism that results at distance and near before proceeding.4 Yoke prisms stronger than about 3.25∆ may interfere with patient comfort and adaptation.
PALS AND SLAB-OFF LINE LOCATION
With bifocals and multifocals, the slab-off line is placed at the top of the seg. When ordering a slab-off for a PAL, your lab will probably place the slab-off line at the PRP unless you specify otherwise. Somewhat lower is usually preferable. It’s important to remember that when the line-of-sight intersects the slab-off line, the patient will experience a monocular diplopia. Since there is no seg line, you have some options in placing the slab-off line.
Recently an ECP reported a case in which the slab-off line (in the left eye) was initially placed at the prism reference point (i.e., 8 mm below the DRP). This interfered with the use of the patient’s outside rearview mirror when he was driving. The solution was to remake the left lens with the same amount of slab-off, but with the line placed several millimeters lower. Testing the placement of the line with a piece of Scotch “misty” tape so the patient can help is usually a good idea.
Another PAL/slab-off issue relates to digital PAL lenses versus conventionally produced PAL lenses. With conventional lenses, the slab-off line must be placed on the side of the lens opposite the location of the add. With back-surface-add digital lenses, some labs are able to place the slab-off on the same side of the lens as the add, and the slab-off line then becomes harder to detect cosmetically. This is partly due to the fact that it is on the back of the lens, and partly due to the fact that it is a bit less well-defined. A pre-cast reverse slab-off can be used, but the line will be more noticeable.
The NOT-SO-APPARENT TRUTH
Although some patients who cannot tolerate their uncorrected imbalance return to have the problem evaluated and corrected, some go elsewhere to seek relief. Others with a smaller amount of vertical imbalance gradually learn to tolerate or partially adapt and ultimately seek other providers for their care.
THE SOLUTION
Use bifocal trial lenses and prisms to demonstrate the effect of eliminating prismatic imbalance when reading. Use your laboratory’s consultants when you have patients with imbalance problems. Do regular progress evaluations to identify patients experiencing problems with adaptation. When you identify a potential problem with vertical imbalance, a slab-off may not be needed, but careful clinical judgment should be exercised. Your staff and especially your patients will appreciate and talk about your meticulous care and concern for their functional vision.
Ask your lab to notify you when an order is placed for PALs or multifocals with vertical imbalances of 1.25 diopters or more. For a PAL with a drop from the DRP to the PRP of 10 mm, and from the PRP to the NRP, a drop of 12 mm and a 1.25 diopter vertical imbalance at the DRP, the unwanted vertical prism would be 1.25∆ at distance and 1.50∆ at near. By prescribing vertical prism for the imbalance at the DRP level and slab-off for the imbalance at the NRP, the patient will have no vertical imbalance for distance at the DRP level and no vertical imbalance at the NRP for reading. The amount of yoke prism at the DRP and NRP will depend on the Rx and could be excessive. Your lab should be able to do these calculations and advise you if the patient’s eyewear qualifies for PAL lenses. In this case, the amount of slab-off can be produced, and the yoke prism must be in a range to which most patients can adapt. Have your staff look at the Rx used in Fig. 2, and ask if it has high potential for trouble (it usually does). Even if slab-off is possible, don’t ignore the alternatives. You, your staff and your lab should screen orders for vertical imbalance. It will reduce errors, remakes and patient frustration, and it’s all part of providing the best in vision care.■
Palmer R. Cook, OD, is director of professional education at Diversified Ophthalmics in Cincinnati, Ohio.
- Vertical prism disparity means the amounts of vertical prism or the directions of their bases are not the same in both eyes. For example: OD 3∆BU and OS 3∆BD has a total vertical prism disparity of 6∆, and OD 3∆BY and 1∆BU has a total vertical prism disparity of 2∆.
- Vertical imbalance means the lens powers are not the same in both the right and left lenses in the vertical (090) meridian.
- The Major Reference Point in a single vision or multifocal lens is the one point in the lens that gives the prescription for distance vision. The closest thing to an MRP in a PAL is the DRP or distance reference point. The DRP for most patients should fall about 3 or 4 mm below the center of the pupil.
- Yoke prisms are prisms of equal power and with their bases in the same direction (Base Up or Base Down and sometimes Base Right or Base Left). Most patients tolerate them fairly well up to about 3.25∆. Many labs recommend restricting their yoke prisms to no more than 2.5∆.













