|
England’s King Henry I (1100 – 1137), recognizing the need for accurate repeatable measurements, decreed that a yard would be the distance from the tip of his nose to the end of his thumb, and other units of measurement were based on that rough and ready standard. We have come a long way since old King Henry, no matter how you measure it. We are in agreement over what an inch or a millimeter represents. But having a reliable standard of measurement is only the beginning when designing eyewear. Properly taking the measurements is the key to designing eyewear that looks good, fits well and gives great vision.
Gross “Measurements”
These aren’t really measurements at all. They are the things you should look at during frame selection so you can guide the patient to the best possible choice. Frames or mountings should give an overall width that is approximately the same as the width of the patient’s face. Using turnback temples and wide DBLs (Distance Between Lenses) with adjustable pads is a valid way of achieving a needed overall width without having an overly large lens size that increases thickness and weight in the higher powers. Temples should be long enough to allow the shaft to rest on the top of the attachment of the patient’s ears to the side of his head without having an excess of the shaft trailing further back along the skull.
Prepare For Measurements
For MRP (Major Reference Points) heights, seg heights and reading levels you must always have the selected frame or mounting in the anticipated wearing position before measuring. This means that the top of the lenses will generally follow the patient’s brow line, the frame will be neither too high nor too low on the face, the vertex distances (right and left) will be equal and the pantoscopic tilt will be appropriate. Anything less will lead to trouble, especially with stronger prescriptions and low tolerance patients.
Careful observation is important to determine the vertical placement of MRPs and to determine the best placement for seg lines and reading levels. Patients may carry their chins high or tucked down or anywhere between these extremes. Patients assuming an unusual head positions as measurements are taken is a common cause for eyewear dissatisfaction. It is only when the frame is in the position in which it will be worn, and when the patient has his chin in his “normal” high, low or in-between orientation that you can obtain a successful measurement. Take a close look at your patient. Is he sitting at the design table, chin up, shoulders squared and waiting expectantly for whatever you are going to do next? If so, you may be set up for measurements that will disappoint.
Pre-measurement Alignment
It is usually a simple matter to: 1. move the bend back if necessary so the temple shaft rests on the attachment of the ear on both sides, 2. adjust the temple-open angle so the vertex distances are equal, 3. level the frame and achieve the correct pantoscopic angle and 4. adjust the pads for a comfortable and symmetrical fit on the nose. After making these preliminary adjustments, you should then quickly review the fit, since every bend you make anywhere on the frame has the potential of affecting the adjustments that you have previously made. Are you ready to take the measurements now? Guess again.

Accuracy requires that the front be in the correct position before you begin measuring. This patient has a right hyper eye. For a better appearance and to minimize the difference in MRP heights (which will help minimize lens thickness) the simulated frame has been tilted downward on the patient’s left and upward on his right. Since most doctors examine patients with hyper eyes with a level refractor, the cylinder axis may need to be compensated (counterclockwise in this case) because the frame is tilted. The heights of the MRPs must be measured from the deepest point of the eyewire.
WHEN THE MEASUREMENT WASN’T RIGHT
Pre-alignment
In this case the right pupil is fairly close to being directly above the deepest point of the eyewire. The left eye has a smaller half-PD (Pupillary Distance), so care must be taken to measure the left MRP height at the deepest point of the eyewire, which is significantly lateral to the pupil. The fit is further complicated by the slope of the midline of the nose, which slopes downward to the patient’s left. Adjustable pads will probably be required for a comfortable fit. Result: Unless the frame is prealigned with a tilt to his left (as shown) and measurements are carefully taken, this patient’s difficulties with new eyewear will vary in direct proportion to the strength of his prescription. With a low power, spherical Rx he may experience adaptation difficulties and some annoying problems that will persist. With a stronger Rx, including an add and a significant amount of cylinder, his eyewear may be unwearable.

Observe Your Patient
Most people look at a point about 17 feet in front of themselves when they walk, so the combination of vertex, pantoscopic angle and MRP placement should allow them to see the ground clearly at about that distance with a normal head position. Also patients may have unusual, characteristic head positioning (turns, tilts, chin tucks) for anatomical, neurological or personal preference reasons. Ask about such apparent eccentricities only after careful observation. Once you call attention to such an anomaly, the patient may compensate or exaggerate to the point that it becomes difficult to determine what is “normal” for them. Measurements should be taken with the patient’s head in whatever is their “normal” position. Your experience, careful thought and skill must all play a role in getting this part of taking measurements exactly right.
The measurements for single-vision prescriptions include the lateral and vertical position of the MRPs. For patients with bifocals or trifocals, a seg height must be taken and patients who require a neutralizing prism (i.e. slab-off) for reading must have a near MRP measured for each eye. The results of incorrect measurements vary depending on the prescription and the patient’s tolerance. When the tolerance is low and the error great, we sometimes receive the mixed blessing of having the patient return, giving us the opportunity to make the needed corrections. If the patient’s dissatisfaction is somewhat less, you may never hear of the problem, but your reputation and practice may suffer.
THINGS THAT MAKE A DIFFERENCE
• When you think your pre-measurement fit is right, always look at the patient from above with their chin tucked in to be sure the frame wrap is correct and that the front approximately parallels the facial plane equally on the right and left sides.
• When you think your pre-measurement fit is right, always look at the patient from both sides to check the pantoscopic tilt and to be sure the shaft of the temple is resting on the top of the attachment of the ear to the head.
• When you think your pre-measurement fit is right, always look at the patient from the front to be sure the pad adjustment is appropriate and that the front is following the brow line as it should when the eyewear is dispensed.
• When providing your patient with prescription half-eye readers, place the edge of the PD ruler in the plane in which the readers will be worn—usually down the nose—and take a near PD as you normally would. Also, if the reading Rx at a normal vertex is over four diopters or so, you should consider doing a power compensation to account for the increase in vertex distance.
Measuring The PD
We have all used a millimeter ruler to measure the interpupillary distance or PD. It is fast, easy, accurate (if done properly), handy and inexpensive. The following general rules apply for accurate distance PDs with a ruler: 1. You must be directly in front of the patient and they should have their eyewear off. 2. Hold the PD rule in your right hand. The scale on the PD rule must fall in the spectacle plane so always use a thin ruler and tilt it so the edge is in the location that the front will occupy. 3. Direct the patient to look at your open (right eye) and occlude the patient’s left eye. 4. Position the rule so that the 0 mark is at the temporal edge of the patient’s limbus and so that the edge of the rule bisects the pupil. 5. Move the occluder to cover the patient’s right eye and direct him to look at your now open left eye. The rule should bisect the patient’s left pupil. 6. Note the mark that falls on the patient’s nasal limbus. For most patients this will be somewhere between 55 and 72 millimeters.
To measure the near PD: 1. You should move so your right eye is in front of the patient’s nose. 2. You must be at the distance that the near correction is designed for—usually a reading distance of about 16 inches. 3. Occlude the patient’s left eye. 4. Position the rule so that the 0 mark is at the temporal edge of the patient’s limbus and so that the edge of the rule bisects the pupil horizontally. If you are measuring a PD for readers, which are typically worn down-the-nose, the edge of the rule should be placed further down the nose. 5. Move the occluder to cover the patient’s right eye and direct him to look at your now open left eye. The rule should bisect the patient’s left pupil. 6. Note the mark that falls on the patient’s nasal limbus. For most patients this will be about three millimeters less than their distance PD.
Half-PDs
The above general rules work well for patients who have pupils that are centered in the iris and which are equidistant from the center of the bridge of the proposed eyewear when looking at a distant object that is directly in front of them. Some patients do not neatly fit this anatomic ideal. For patients whose nose drifts to the right or left (i.e. the midline of the nose is not vertical), or for those whose pupillary centers are not equidistant from the midline of their noses the PD should be measured from the center of the pupil to the midline of the previously adjusted frame. By marking the center of the bridge and then using that mark as a guideline with the frame in place you can put a small mark (with an eyebrow pencil or other non-indelible marker) on the patient’s nose at the pupillary level on the frame’s midline to eliminate any error that might be induced by the lower portion of the nose being significantly to the right or left of the midline of the root of the nose. The general rules, one to three, are the same as above, but for a half-PD measurement the 0 mark of the ruler (see “4” above) is placed at the center of the pupil of the right eye. The right half-PD is then read at the mark on the patient’s nose. The occluder is then moved to cover the right eye and the patient is directed to look at your now open left eye. Note the mark that falls on the center of the patient’s left pupil. Subtracting the right half-PD from this will give the left half-PD. Don’t forget to remove the mark from the patient’s nose if you had to use one.
WHEN THE MEASUREMENT WASN’T RIGHT
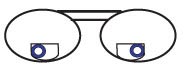
Near PD
The measured near PD is too narrow. If the patient looks to his right his right pupil will intersect the side of the right seg after moving only three or four millimeters or so and the patient will experience a bi-prism effect which may be interpreted as doubling or blur. On looking to the left, the left pupil will intersect the side of the left seg after moving only three or four millimeters, again giving doubling or blur. The same thing happens if the segs are too far apart. Result: The patient has been given a very narrow lateral field and will have to keep re-pointing his nose as he reads across all but the narrowest columns of print. Ideally the lines of sight (represented by the centers of the pupils) should be centered in the segs when looking at print directly in front of him. The same narrowing of the near field of vision occurs with PALs when the location of the reading area is too narrow or too far apart.
Unequal Half-PDs
Geometric Centers of the Eyewires
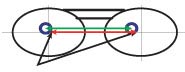
MRP Locations
The patient has unequal half-PDs, but the MRPs were placed as though the pupils were equidistant from the midline of the frame. The red and green arrows are both the same length as the patient’s PD. The MRPs were placed on the mounting line and decentered inward an equal amount in each eye. Result: Because the separation of the MRPs is the same as the patient’s anatomical PD, the patient can turn his head (to the right in this case) to view through the optical centers simultaneously. In the straight-ahead position (shown above) the patient will have the disadvantages of off-optical- center viewing. He may have unwanted lateral and even vertical prism if the Rx contains cylinder with an oblique axis.
LT
Palmer R. Cook, OD is director of education for Diversified Ophthalmics in Cincinnati.
Next Month: More about measurements and what can go wrong, including MRP heights, seg heights and some “Easy To Overlook Errors & Their Results.”
|


















