
By Palmer R. Cook, OD
Whether you call them monocular pds or half pds, they are a refinement in data gathering that can help you supply better performing eyewear to your patients. Monocular pds are important. They are part of the data that should be used in designing high performance prescription eyewear. But too often the full message in the patient’s monocular pd data is misunderstood, ignored or downright incorrect. This can lead to poor lens performance, discomfort, patient dissatisfaction and dispenser despair.
WHAT ARE MONOCULAR PDS?
It is important to understand exactly what the term monocular pd means. A common misperception is that a monocular pd is the distance from the center of the pupil (right or left) to the center of the patient’s bridge when the patient’s head is in the primary or “straight ahead” position, and the object of regard is at a far distance. Actually the measurement is from the point where the line-of-sight intersects the lens to the center of the bridge of the frame.
Monocular pd measurements are data for the fabrication of eyewear and must relate to the frame. Fortunately the center of the patient’s bridge and the center of the frame’s bridge generally coincide. Even when they do not coincide, the difference may be small and with a midrange or lower prescription power, the finished eyewear is usable. When the slope of one side of the nose is steeper, if one side of the nose bulges more than the other, or if the nose is not centered right-to-left, a frame with fixed pads will be shifted to one side. The solution in such a case is to use a frame with adjustable pads and compensate the best you can for a functional and cosmetic success. In almost every case the widest part of the eyewear should be as wide as the patient’s face, and it should be centered. Even if the nose is symmetrical and centered, the eyes may not be equidistant from the centerline of the nose.
ANATOMICAL VARIATIONS
Anything is possible. The nose or the glabella (i.e., the area between the eyebrows at the root of the nose) may or may not be centered relative to the sides of the head. The eyes may or may not be equidistant from the center of the glabella. The ridge of the nose may descend from the glabella either straight down or at an angle, and the sides of the nose may or may not slope equally away from the ridge of the nose.
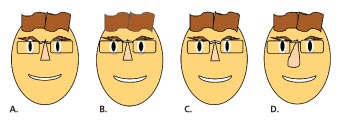
A. Nose centered: Easy to fit. The monocular pds are equal, and the frame will center on the face.
B. Nose off-center to patient’s right: Adjustable pads or a build-up of the left pad on a fixed frame center the frame better on the face. Only after the frame is fitted can the monocular pds be measured.
C. Nose centered: Patient’s left monocular pd is smaller than his right monocular pd. The monocular pds are unequal and the left MRP must be decentered inward more than the right.
D. Glabella centered, nose slopes to right: The frame is pushed to the patient’s right. Adjustable pads are needed or wedge build-up pads may allow the frame to be centered better on the face. Only after the frame is fitted can the monocular pds be measured.
No matter what anatomical variation is present, you must first adjust the frame before taking the monocular pd. Then mark the center of the bridge of the frame. This allows you to take the monocular pd from the center of the pupil to the mark you placed on the center of the bridge.
If you use a pupilometer to measure monocular pds, look for a raised marker on the top of the instrument indicating the center of measurements. Place an arrow sticker, like those used to indicate where signatures go on documents, to mark the location of the raised marker (i.e., the patient’s glabella). After taking the monocular pds, the location of the center dot on the fitted frame must be compared to the location of the center of the patient’s glabella. If the displacement of the dot on the frame is 2 mm to the patient’s right of the center of their glabella, then you must add 2 mm to the patient’s right monocular pd and subtract 2 mm from the left monocular pd. If the displacement is to the patient’s left, the amount of displacement must be subtracted from the patient’s right monocular pd and added to the patient’s left monocular pd.
NEAR MONOCULAR PDS
Although a distance pd is usually taken in the spectacle plane, it is the same at any distance from the corneas. This is not true of near pds (or near monocular pds). The distance between the converging lines-of-sight varies depending on the vertex distance. Ideally, the lines-of-sight should be centered in the corridors when viewing at intermediate distances and when centered in the reading area when viewing at near. For people wearing bifocals, multifocals and PALs, the near vertex measurement is typically longer than the distance vertex measurement. By varying the pantoscopic tilt you are effectively varying the distance between the lines-of-sight when viewing at intermediate and near distances. Near pds vary according to the width of the distance pd and the near viewing distance (see Table 1) as well as according to the near vertex distance.
Working Distances 25 cm, 33.3 cm, 40 cm
|
| Distance PD Near PDs | ||
|---|---|---|---|
| 74 | 67.0 | 68.5 | 69.5 |
| 72 | 65.0 | 66.5 | 67.5 |
| 70 | 63.0 | 65.0 | 65.5 |
| 68 | 61.5 | 63.0 | 63.5 |
| 66 | 59.5 | 61.0 | 62.0 |
| 64 | 58.0 | 59.0 | 60.0 |
| 62 | 56.0 | 57.0 | 58.0 |
| 60 | 54.0 | 55.5 | 56.0 |
| 58 | 52.5 | 53.5 | 54.0 |
| 56 | 50.5 | 52.0 | 52.5 |
| 54 | 48.5 | 50.0 | 50.5 |
| Table 1. These near pds are assuming a 13.5 distance from the center of rotation of the eye and a 13.5 vertex distance. If your patient looks down 29 degrees from the distance reference point to the near reference point, the vertex distance is increased to about 17.4 mm, and the near pd which measures 56 mm at a 13.5 vertex distance is now decreased to about 52 mm for a 40 cm viewing distance. | |||
EFFECT OF PANTOSCOPIC TILT
Increasing pantoscopic tilt effectively increases the width of both the reading area of a PAL and the width of the corridor. Increasing pantoscopic tilt also effectively increases the separation of the lines-of-sight at the point they pass through the lenses for near viewing. Decreasing the pantoscopic tilt narrows the width of the corridors and reading areas, and it also narrows the patient’s near pd.
Obviously, adjusting the pantoscopic tilt is extremely important when fitting progressive lenses. Unlike single vision, and to some extent multifocals, the purpose of pantoscopic tilt is more than just keeping the lines of sight at right angles to the lens surfaces. With non-individualized progressives, manufacturers set a default value for the separation of the centers of the reading zones. It is up to you to find the pantoscopic angle that works best for your patient.
With individualized (free-form) lenses you specify the pantoscopic angle, vertex distance and wrap, and digital lens production incorporates your data into the lenses. The result of using accurate monocular pds and individualized lenses helps keep the patient’s lines-of-sight equally centered for better performance at near and intermediate distances.
WHAT HAPPENS IF...
Experiment for Yourself
To experience the amount of change in head position a patient must make if you shift the MRPs 2 millimeters to the right or left for a better lens outcome, place a vertical two millimeter wide strip of tape on one of your own lenses – then look at a distant point, first from the right side of the tape, then turn your head so you are looking just to the left of the tape.
If your monocular pds are incorrect, but if they total the patient’s distance pd, the patient will only have to position his head a bit to the left or to the right to achieve full use of the corridors and reading areas. If the monocular pd total is greater or less than the true distance binocular pd, the width of the reading areas and the width of the corridors will be narrowed by about 2 mm for every 1 mm of error.
If the monocular pds differ by even as little as 2 mm, you may have a problem with excessive thickness on the side that requires the most decentration. It’s easy to compute the amount of decentration needed. Just add the A measurement and the DBL, and divide by two (e.g., a 50a20 frame has a total frame pd of 50+20 or 70. Dividing this by two gives you the frame half pd, 35).
In most cases the patient’s full pd should be 1 to 3 mm smaller than the frame pd. Each monocular pd can be subtracted from the frame half pd to determine the needed decentration. The inequality in monocular pds and the needed decentration in each eye can add up to problems. Of course with higher powers and larger lens sizes, the issues become much more troublesome. When in doubt, call your lab for suggestions.
THIS DIDN’T WORK
 The patient’s full pd was 64 and the monocular pds were OD 30 and OS 34. The Rx was +8.00 OU. The chosen frame was a 56-18-140. The selected lens material was standard plastic. Because of the high power of the lenses, the order specified that the edge thickness be kept to a minimum. The alarm bells should be going off at this point.
The patient’s full pd was 64 and the monocular pds were OD 30 and OS 34. The Rx was +8.00 OU. The chosen frame was a 56-18-140. The selected lens material was standard plastic. Because of the high power of the lenses, the order specified that the edge thickness be kept to a minimum. The alarm bells should be going off at this point.
The patient’s full pd was 64 and the frame pd is 74. If the patient had equal monocular pds, the lens optical centers would be decentered (i.e., moved inward) by 5 mm in each eye. Since the patient’s monocular pds are 30 and 34, the right lens had to be decentered 7 mm inward and the left had to be decentered inward 3 mm. As requested the edge thickness was kept to a minimum, but the left lens center thickness had to be increased to allow enough lens material to fill the large eyesize. The right lens center thickness is 13.5 mm and weighs 20.95 gm, the left is 9.6 mm thick and weighs 15.71 gm—nearly a 25 percent difference in weight. The maximum edge thickness difference is obvious. The patient refused to accept the eyewear at dispensing.
By remaking the lenses with equal monocular pds of 32 and using the full pd of 64, the lens thicknesses, magnification and weight differences were equalized. Since moving the line-of-sight 1 mm is about a 2 degree change in eye orientation, the accommodation that the patient has to make is to turn his head to move his lines-of-sight approximately 4 degrees to his left. This is less than the angle the minute hand on a clock moves in going from 12 o’clock to one minute after 12.
Of course using a smaller eyesize and bridge size, and a higher index lens material would help. With a 1.60 material the thicknesses would be reduced by about 17 percent and if using 1.67 the reduction would be about 24 percent, but the magnification difference would remain high enough to potentially elicit aniseikonic symptoms.
HEAD TURNS
Not all patients hold their head like a Marine standing at attention. Some patients typically have a head turn (sometimes called “cape”) to the right or left as they look straight ahead. When taking monocular pds in such a case, the patient, with his head turned to its “normal” position should be seated in front of the technician. In this case the technician’s nose should be pointed directly at the patient, but the patient’s nose will be pointed a bit to the left or right. A pd rule should be held parallel to your facial plane. The resulting monocular pd findings can help your patient get the best performance from his new eyewear.

Whether you use sophisticated measuring devices or simply a pd rule, careful observation is needed to determine if a head turn is present. One technique is to hand the patient a reading card, asking that it be held in both hands. If a head turn is present, this usually will reveal it. Looking at some snapshots of the patient or their picture on an ID card or driver’s license can be helpful. Another technique is to seat the patient and position their head so that it is straight, then ask them to read an eye chart from the larger letters down. Patients who have a true head turn will turn to their habitual head position as they try to read the smaller letters. This is a highly repeatable test. In no case should you call your patient’s attention to your suspicion of a head turn until you have completed your observations. If the head turn causes extremely different monocular pds and complications in lens and eyewear design, give careful thought as to whether the monocular pds could be partially or wholly equalized for a better outcome. In any case, if the monocular pds are modified, they should total the full anatomical pd. If a head turn results in the lines-of-sight passing through strong lenses at an angle, the Martin formulae for tilted optics should be applied. Your laboratory should be able to help with this.
The accurate lateral and vertical placement of MRPs becomes exponentially more critical: 1. As the power of the Rx increases. 2. If an add (particularly a progressive) is needed or 3. Whenever aspheric lenses are used. Clinical judgment and experience on the part of the optometrist and/or optician in assessing the patient’s anatomy is extremely important in these cases to ensure that comfortable and well performing eyewear is dispensed.
Clinical Tips
Clinical Tip When fitting multifocals, especially in higher powered Rxs, although you normally place the MRPs or optical centers at unequal decentrations to agree with unequal monocular pds, you may wish to equalize the decentration of the segs for a better cosmetic result. This will require the patient to turn his head slightly for reading if he is to have the benefit of the full width of the seg.
Clinical Tip Patients who have lost an eye tend to carry their heads turned somewhat to the side of the lost eye. This should be taken into account when measuring the monocular pd by taking the pd with a pd rule with the patient’s head in its slightly turned position.
Clinical Tip When the decentration needed to meet the monocular pd requirements looks like it might be a problem, try decreasing the eyesize, using turnback temples to get the needed eyewear width. This can significantly decrease thickness and magnification problems.
Clinical Tip You can increase the effective width of both the corridor and the reading area of a progressive lens by using more illumination. This decreases the pupil sizes and increases the depth of focus of the eyes. It is a temporary measure that helps in adaptation, especially if the patient has not previously worn PAL lenses.
Clinical Tip If the frame of choice has a temple attachment at the top of the eyewire, the available range for changing the near vertex distance is twice as great as it would be if the temple attachment were halfway from the top of the lens to the bottom. This is especially important to keep in mind when fitting first-time progressive lens wearers or difficult to fit patients.
Clinical Tip It’s good technique to take a careful full (i.e., binocular) distance pd, and then add the monocular pds to be sure the total is the same as the distance pd. Remeasure as needed if the total doesn’t match. In every case the separation of the distance MRPs and the patient’s full pd (i.e., the sum of the distance monocular pds) must be equal.
Palmer R. Cook, OD, is director of professional education at Diversified Ophthalmics, Cincinnati, Ohio.













