Coping With Corridors
By Barry Santini, ABOM
Release Date: September 1, 2015
Expiration Date: June 1, 2020
Learning Objectives:
Upon completion of this program, the participant should be able to:
- Understand what opportunities are present for specifying progressive lens corridor lengths.
- Know when a specific corridor length is required.
- Learn the lenses and options when a specific corridor length is a requirement.
Faculty/Editorial Board:
 Barry Santini, ABOM, graduated from New York Technical College in 1975 with an AAS in Ophthalmic Dispensing. He is a New York State licensed optician with contact lens certification, is ABO certified and was awarded an ABO Master in 1994. As sales manager for Tele Vue Optics from 1987 to 2003, Santini developed his knowledge of precision optics and has been an owner of Long Island Opticians in Seaford N.Y., from 1996 to present. In addition, Santini is an amatuer astronomer and lecturer and plays bass trombone in the Brooklyn Symphony.
Barry Santini, ABOM, graduated from New York Technical College in 1975 with an AAS in Ophthalmic Dispensing. He is a New York State licensed optician with contact lens certification, is ABO certified and was awarded an ABO Master in 1994. As sales manager for Tele Vue Optics from 1987 to 2003, Santini developed his knowledge of precision optics and has been an owner of Long Island Opticians in Seaford N.Y., from 1996 to present. In addition, Santini is an amatuer astronomer and lecturer and plays bass trombone in the Brooklyn Symphony.
Credit Statement:
This course is approved for one (1) hour of Technical, Level II CE credit by the American Board of Opticianry (ABO). Course STWJM614-2
INTRODUCTION
In the new millennium, as free-form manufacturing overcame the economic and logistic limitations imposed by traditional progressive production, a cornucopia of lens design choices unfolded on the optical market. Through software-based, free-form design, manufacturers could now offer lenses of variable design priorities, where the optician could now specify not only which utility area was most important, but also the length and even slope of the progressive corridor. And the most advanced designs featured a variable corridor, which would individually tailor the progressive to fit the chosen frame. However, this approach can come with a downside, with patients sometimes encountering difficulty adjusting to different reading levels resulting from the design software adjusting corridor length differently between smaller dress and larger-sized sunwear styles. The challenge to be taken up by today's optician is to recognize how much more involved they need to be in designing lenses that will satisfy the expectations of their customers.
OLD VERSUS NEW CHALLENGES
Since the introduction of Varilux, the first progressive addition lens in 1959, eyecare professionals have faced numerous challenges in learning to fit these types of lenses. Clearly, success with progressives has always been about obtaining a type of magical balance between sometimes conflicting elements, including acuity, comfort, utility, perceptual and postural adaptation, in addition to business concerns centered on price and perceived value.
Until recently, ECPs have lacked the ability to tailor specific or overall aspects of a progressive lens' design, including its basic design philosophy, i.e., merit weighting of aberrations, surface astigmatism, power errors or corridor length. Consequently, they had resigned themselves to the reality that obtaining patient satisfaction would be limited only to manipulating height, design, add power or specific brand. Progressive lens fitting was seen as a risk-filled and serendipitous endeavor, often accompanied by expensive trial and error lens remakes and loss of patient trust.
Today, the advent of free-form lens production technology has now given ECPs tools that had previously been strictly within the province of the original lens designer. The proper use of these tools—most importantly the ability to specify progressive corridor length—now requires eyecare professionals to possess an in-depth understanding of the interplay between the eye's natural reading level preferences, lens fitting parameters, individual prescription values and critically, even the design goals of the lens itself.
Therefore, it is essential for ECPs to comprehensively understand the history, design, vocabulary, definitions, fitting concepts and Rx considerations involved in the fitting of progressive lenses, and the impact that choosing the ideal corridor length has on improving satisfaction, increasing trust and elevating your professional credibility in the eyes of your client.
THE CHALLENGE OF PROGRESSIVE DESIGN
Although the invention of progressive addition lenses was first described in 1907, another 50 years would pass until Bernard Maitenaz of Essel, a forerunner of Essilor, engineered a way to commercially produce progressive lenses. Even as the hurdles of making lenses with a seamless transition between distance and reading were overcome, European opticians—long trained to prize optical quality above everything else—found themselves reluctant to embrace a new lens technology that appeared to increase optical errors rather than decrease them.
In the first decades of progressive development, lens designers found that the easiest way to decrease surface astigmatism and distortion was to spread out the progressive gradient by making the progressive corridor as long as possible. This is the origin of why many ECPs favor longer corridor designs. But two problems can accompany this approach: 1. The reading level can end up uncomfortably low, and 2. Different frame "B" sizes may result in different reading levels. Here, wearers often experience discomfort and adaptation problems switch between pairs. This is, in fact, a problem we often encounter today.
The defacto challenge facing progressive design was thus defined: How do we strike the optimal balance between comfort, acuity and utility for each prescription, wearer and frame style? The answer begins with defining a common, working vocabulary of basic progressive terms and fitting concepts.
UNDERSTANDING PROGRESSIVE BASICS
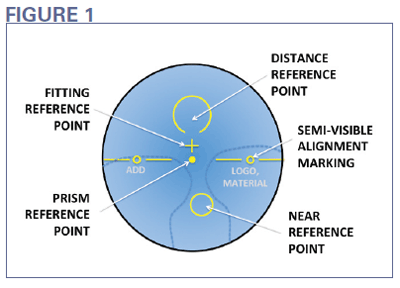 Unlike bifocal lenses, which have only two zones of vision and a sharp line marking the border between them, progressive lenses have many reference points that need to be considered. Below are the major cardinal points common to every progressive lens and their respective definitions:
Unlike bifocal lenses, which have only two zones of vision and a sharp line marking the border between them, progressive lenses have many reference points that need to be considered. Below are the major cardinal points common to every progressive lens and their respective definitions:
Fitting Point: The reference point at which the design's fitting cross is placed. The com mon orthodoxy is to place the Fitting Point at the center of the eye's pupil while the patient's facial plane is in their natural position, i.e., normal posture. Often overlooked is that the progressive power gradient, i.e., the corridor, just begins its slope at the Fitting Point. In the most modern designs, this change is slow for the first 2 to 4 mm.
Major Reference Point (MRP): These are the lens designer's points of reference for optical calculation and alignment. The MRP is also the point for measuring prism in both an unmounted lens and a finished pair of eyewear. Some brands refer to the MRP as the PRP or Prism Reference Point.
Alignment Reference Markings: These engraved reference points, 34 mm apart, 17 mm each side of the MRP, are used for aligning the progressive lens during finishing, as well as for verifying correct prescription axis and placement in a pair of finished eyewear.
Progressive Drop: The distance between the Fitting Point and the MRP/Alignment Reference Marks. This value varies between different manufacturers and even different designs within a manufacturer's lens portfolio. It can range from 0 to 6 mm, with 4 mm being the most commonly encountered value.
Near Reference Point: The area outlined for verifying the reading Rx power.
Distance Reference Point: The area outlined for verifying the distance Rx power, generally located approximately 4 mm above the Fitting Point, providing an area completely free of the progressive power gradient.
FITTING CONCEPTS IN MODERN PROGRESSIVES
Below are the definitions and fitting concepts needed to be understood by ECPs in order to fully grasp the mechanics of defining and choosing corridor length:
Corridor Length: The linear distance between the beginning of the power gradient—the Fitting Point—and the target add value, most commonly defined as 85 percent of add power.
Target Add Value: Variably classed as either 85, 95 or 100 percent of the prescribed add value, depending on the design. Manufacturers are free to define corridor lengths using either of these target add values. It is therefore important to contact the manufacturer and learn which value they use when you are comparing corridor lengths between different designs. Rule of thumb: Add approximately 2 mm to the corridor length of an 85 percent target add value design when comparing corridor lengths with a 100 percent target value design.
Minimum Reading Area: Experience has shown that a progressive reading area should be a minimum of 4 mm to 5 mm in height. Many traditional short corridor designs may provide as little as 3 to 4 mm, which can result in compromised utility and comfort in the reading and intermediate areas.
Minimum Fitting Height: The distance from the Fitting Point to the center of the reading area. Depending upon the manufacturer or design, targeting the Minimum Fitting Height can truncate up to half of the available reading area. A general recommendation is to choose a frame that allows the addition of between 2 mm and 4 mm to the Minimum Fitting Height. Doing so will ensure the wearer has the minimally-comfortable reading utility.
CHOOSING CORRIDOR LENGTH
To begin the choice of a corridor length, start with your fitting height, and subtract 4 mm to 5 mm, which allocates enough height for a minimum useful reading area. The difference left is a good approximate number to begin determining your target corridor length.
Here's an example:
For a fitting height of 18 mm, corridor length roughly calculates as follows: 18 mm minus 4 mm (minimum reading area height) = a 14 mm Corridor Length Value
Tip: Your calculated corridor length value may not always be obtainable in a specific progressive design. Therefore, always keep the minimum useful reading area in mind as you select the next closest corridor available.
In the above example, if the design selected only provides a choice between an 8 mm or 10 mm corridor, the final value chosen will depend upon these additional considerations:
Total Frame Height and Contour: Frame style, size and shape may dictate an adjustment to your target corridor length to ensure the full reading area is not truncated by the contour of the frame's lower rim. Pupillary distance also places a role here, with narrower PDs more sensitive to being truncated by the upward slope of the frame's nasal eyewire.
Vertex Distance: Closer vertex distances require shorter corridors to compensate for the reduced drop of the eye's declination intercept with the lens surface. And vice versa for long vertex distances, which then may need longer corridors.
Pantoscopic Angle: Greater pantoscopic angles require shorter corridors, and lesser pantoscopic angles require longer corridors for the same conceptual reason stated above in vertex distance.
Rule of thumb: Every 1-mm increase in corridor length will require approximately a 2-degree increase in eye declination.
Tip: The less accommodation reserve, i.e., increasing age, the quicker the wearer will need to get to the target reading add.
RX CONSIDERATIONS
Prescription considerations can influence your selection of corridor length:
Total Add Power: Higher add powers—greater than 2.25D—feature smaller reading and narrower intermediate areas and more surface astigmatism. Therefore, a too short corridor may deliver unacceptable optics because of increased surface astigmatism.
Rx Delta: Total power change seen in a new Rx should be considered for its impact on both distance vision clarity and reading declination. The direction of change, more plus or less plus, is important to factor in as well, regardless of the specific type of ametropia.
Ametropic Error: Spectacle magnification and prism may impact your corridor choice. The minified and upwardly displaced image in a myopic Rx requires consideration of selecting a shorter value for the corridor. For hyperopic prescriptions, because of image magnification and base up prism, the opposite is true.
Center of Rotation and Dioptric Error: Hyperopic eyes have shorter axial lengths, while myopic eyes feature longer axial lengths. These axial length differences place the center of rotation of hyperopic eyes closer to the cornea, while in myopic eyes the CR further away. This, along with the fitted vertex distance, can influence the actual point where the visual axis intersects the lens when the eye rotates downward for the near gaze point.
Prism Thinning: If base down thinning prism is present, it will upwardly deviate the image at near. In higher adds, this results in a noticeable decrease of the required eye depression angle for the wearer and is important to keep in mind as you determine corridor length.
Lens Design Priority: The basic design priority of the lens, i.e., whether the distance, intermediate or reading area has been targeted to be most important, can further impact your corridor value calculation. For example, a client with a plano DV/+2.00D add may state a preference for clear, edge-to-edge distance vision. Choosing a lens design with this as a top priority, but mated to a frame with a short fitting height, illustrates the dilemma of trying to optimize a progressive lens to both a patient's wishes and their chosen frame style.
Non-Linear Progressive Power Gradient: Traditional progressives have featured a linear slope of increasing power. Newer, special designs, optimized for computer and users of mobile devices, deliver a non-linear corridor power gradient, with the top portion of the corridor featuring a faster increase in power. Some wearer's may complain these designs intrude on their DV acuity when they are switching from a traditional or balanced design. Compounding factors here include patient posture and the amount and direction of the prescription change.
COPING WITH CORRIDORS
In traditional progressive lenses, the designer defines a series of performance goals, including a target corridor length and reading add, fixed lens areas, along with a merit weighting of various optical errors, and then enters into an iterative process to figure out which elements of progressive surface should be manipulated to achieve these goals.
Twenty years ago, when frame fashion took a left turn into small B dimensions, manufacturers responded with new, "shorter" corridor versions of their best-selling designs. For years afterward, ECPs often had only the choice between a normal, longer corridor design, or a compact, shorter corridor design. The optics of these early compact offerings, designed for fitting heights of 15 mm and less, were limited by the production constraints imposed by the manufacture of traditional molded surfaces. Often they were significantly compromised by poor peripheral acuity, inadequate intermediate utility, excessive swim and insufficient reading comfort, and therefore were only selected when fitting requirements absolutely demanded. Although manufacturers could have produced a series of separate lenses with stepped corridor options, the economics of manufacturing and inventorying such an expanded series, further compounded by material and feature options, dictated a market reality where offering two corridor versions became the norm.
VARIABLE VERSUS FIXED CORRIDOR DESIGN
Knowing when to use a variable corridor versus a fixed corridor design is both a powerful and useful tool. The main distinction is that variable designs are often used to prioritize the quality of the distance/intermediate area, and fixed designs are used for prioritizing the reading area:
Variable Corridor Designs: Variable designs allow the ECP to adjust the corridor length as they desire. Longer corridors soften the progressive gradient across the lens, resulting in lower surface astigmatism. Benefits can include improved peripheral vision and an increase in the width of the intermediate and reading areas.
Fixed Corridor Designs: Fixed designs are used when prioritizing the size of the reading zone and/or the amount of eye declination required to reach the target add power. Fixed designs excel when fitting a mature add bifocal wearer—greater than 2.25D add—with their first progressive lens.
Fitting pearl: Bifocal wearers, fitted with segments set 8 mm to 9 mm below pupil, are well-suited to using a 10 mm to 12 mm corridor referenced to a 95 to 100 percent target add value. (You're not still fitting bifocal segments using people's lower lids, without noting how far below their pupil the segment line is, are you?)
UNDERSTANDING THE EFFECTS OF GAZE ANGLES AND POSTUREResearch to assess the normal resting and reading positions of the human eye has been extensively carried out by many lens companies and has revealed the following information: DISTANCE VISION GAZE: The primary gaze angle of the eye looking straight is generally referenced to the facial plane, defined as the line that connects the brow, upper and lower orbital bones and the jaw. For a typical distance gaze discussion, the facial plane is considered perpendicular to the floor, thereby providing a distance gaze angle of 0 degree. However, depending on the fit of the chosen frame, the pantoscopic tilt of the lenses may lie at a different angular value. Careful attention must be paid to both the patient's posture and how the fitter's technique may be affecting the measured value (see "The Problem with Posture"). And while the actual progressive transition does begin at the Fitting Point, the initial power gradient here generally does not exceed 0.25D until 3 mm to 4 mm below the FP. This helps ensure wearer comfort and acuity within the common range of head/posture-influenced facial plane angles. READING VISION GAZE: The typical gaze angles for comfortable reading range from 25 to 32 degrees, with the average value assumed to be 30 degrees. This range corresponds to an area on the spectacle lens between 12.5 mm to 16 mm below the FP, fitted with a pantoscopic tilt of 8 degrees. But the actual near gaze angle can be influenced by the wearer's actual facial plane angle when reading, influenced by fixation distance, accommodation/convergence demand, natural posture, reading height preference, occupation, motility restrictions or simple wearer habit. It is therefore essential for the eyecare professional to be alert and analytical in determining a person's actual near gaze angle as they work or read. THE PROBLEM WITH POSTUREIn view of the above, it should be clear that one of the most confounding elements of corridor selection is the need to assess a patient's normal head and neck posture. This is exacerbated by the truncated time available with the patient during selection of a pair of eyewear. From the moment you initially greet a client, try to ascertain if their natural posture is normal or compensatory, using the following guidelines: NORMAL POSTURAL HABIT: The normal head posture of the wearer. COMPENSATORY POSTURAL HABIT: Depending upon how their current glasses have been measured, fitted or the need for a prescription change, a wearer may have developed a compensatory modification of their normal head posture in order to obtain better acuity for driving, using a computer or for reading. For example, a new Rx could reveal a change which effectively adds more plus power. This wearer may seem to exhibit an upward head tilt, developed over time, to compensate and adapt their present Rx for better reading, intermediate or distance clarity. If the patient in question is also known to have trouble adapting to prescription changes, an ECP might consider fitting the new progressive slightly lower than the normal pupil reference/ Fitting Point, thereby attempting to accommodate this posture habit. Then, using a shorter corridor design, ensure a comfortable eye depression angle for reading. It is important to keep the frame's B size and the minimum recommended reading height in mind here when choosing the final corridor length. TIP: Knowing when to ask a patient to learn to use their glasses by adapting their posture habit is just as important as knowing when not to. Time and experience are your friends here, and ECPs should avoid creating strict rules based on a few exceptional experiences. |
USING THE ADVANCED VARIABLE CORRIDOR
If you are ever intimidated or overwhelmed by the idea of juggling all the above factors in order to arrive at an optimal corridor length, then you can always consider selecting one of the advanced, premium class fully-optimized designs. These fully-personalized position of wear designs will automatically take all of the variables into account to strike an ideal balance between distance, intermediate and reading in selecting the final corridor length. You can maximize the customization by uploading the actual frame tracing, along with all the known position of wear variables. More advanced designs promise even greater wearer satisfaction by factoring in the wearer's previous lens design, corridor length, prescription, as well as center of rotation, eye dominance and head cape, if known. These highly customized designs may also feature the ability for dispensers to tweak the final reading height and corridor length by choosing from one of a variety of design priorities, including balanced, distance, intermediate or near.
FINDING THE MAGIC
The greatest challenge in progressive fitting remains the expert integration and assessment of an individual's posture, prescription, needs and wants, and mating that to a chosen lens design and frame style. As we begin to unleash the power of the corridor "genie," eyecare professionals can finally access one of the most powerful tools at their disposal for the fitting of progressive lenses. Don't remain a novice in your understanding of corridors, and have complaining patients swirling about your waiting room. Use the power of choosing corridor length to harmonize patient, prescription and lens design to frame choice. As patients discover the magic of true progressive satisfaction, so will your bottom line.



