Now that you have your COVID-19 team experts reporting on the measures to implement at restart, what exactly are those measures? To what degree do we change our procedures? Let me tell you what we did in our clinics.
Employee and Patient Screenings
While making their appointments, we ask the three magic questions recommended by the CDC:
Have you been in contact with anyone with coronavirus for an extended period without PPE?
Have you recently traveled to a high-risk area?
Have you been sick with fever, cough, or shortness of breath?
If the patient answers yes to any one of these, schedule them 14 days out, and chart the encounter. Ask specifics about their answers, dates, and remedies.
Tell your employees, “If you are sick, stay home.” That should be easy, but in practice, not so much. Employees must answer three questions. In fact, we have them self-certify every day with the following form, as described by the CDC. The Safety Monitor stationed at the ONLY entry door (no back door entry) will fill out the employee assessment.
Daily Employee Assessment
NOTE: ALL FIELDS ARE REQUIRED. Forms will be filed and managed by the Safety Monitor.
Name (First and Last): _________________________________________________________
Employee Location: _________________________ Date and time: _______________________
1) Have you been exposed (which means being within 6 feet for 10 minutes or more without a facemask) to a person with confirmed or probable diagnosis of COVID-19 within the past 14 days? This includes household members, intimate partner or providing care in a household without using recommended infection control precautions.
YES
NO
2) Have you had contact with a person with a confirmed diagnosis of COVID-19, but have not been in close personal contact with them (within 6 feet for 10 minutes or more without a face mask) within the past 14 days?
YES
NO
3) Have you experienced any of the following NEW symptoms in the past 72 hours: fever greater than 100° F / 38° C, new abnormal cough, loss of taste/smell, shortness of breath, diarrhea or flu-like symptoms like body aches? All EMPLOYEES WILL HAVE TEMPERATURE TAKEN WITH TOUCHLESS THERMOMETER TO CONFIRM ACCEPTABLE TEMPERATURE.
Temp. Reading: _________ YES
NO
4) Check the appropriate final response for the day:
Yes to #1 or #3 DO NOT REPORT TO WORK
Call HR and follow standard procedures by calling the attendance line for reporting your absence and follow the guidance for self-quarantine and return to work.
Yes to #2, No to 1 & 3 CLEARED FOR WORK
You must wear a mask at work. Must closely monitor for temperature daily and/or any symptoms. If any symptoms develop, do not come to work and notify HR and call attendance line as outlined above.
All No Responses CLEARED FOR WORK
Mask required while working.
The Safety Monitor will also fill out the form in Figure 1 below. This person will screen the temperature of each employee and patient; recording it with the time they arrived. As patients and employees leave, record that time as well. This way you have a written record of the total number of bodies in the office at one time.
Pro Tip: The Safety Monitor is an excellent position for a new hire. You can train them for the job in a very short time, and they can observe the workings of the clinic without adversely affecting productivity.
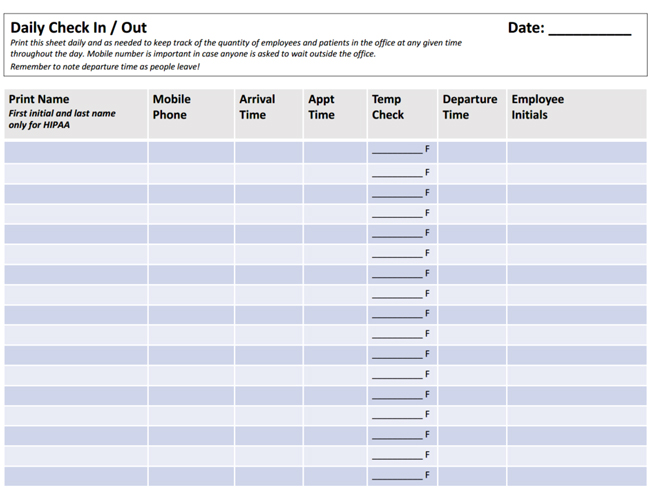 |
According to the CDC and AAO, we choose 100.1OF as the magic temperature number to disallow entry into the clinic. If an employee comes to work and tests higher, we send them home, and they cannot return without a doctor’s release.
If we are at capacity when a patient arrives for an appointment, the Safety Monitor will have them wait in their car and call or otherwise signal them when they may enter. We take a cell number for each patient upon arrival at the Safety Monitor to check in.
Patients must arrive alone to limit the number of people in the office. There are patients, minors, and others, who will need someone with them. Remember to test and document each patient, caregiver, parent, or guardian.
PPE
Here we took the CDC advice for training. We linked their PPE donning and doffing training to our Learning Management system. This way we ensure that all our staff has the same training. We require all employees to wear a surgical mask at work. We do not allow homemade masks in the clinical, front desk, and dispensing areas, but do in the back-office settings. N95 respirators are not required in our offices, and we do not provide them. Employees can wear them if they wish. They throw each mask away at their lunch break and put on a new one before returning to work in the afternoon.
 |  | |
Figure 2: Surgical mask. | Figure 3: Homemade mask |
Our employees will wear gloves in direct patient contact and dispose of them between each patient. This is advice from both the AOA, AAO, ABO, and NAO, and includes clinical workup, adjustments and dispensing, but not contact lens insertion and removal training according to the ABO and AOA. Cleaning hands with soap and water are what we need here. Hand sanitizer would not suffice because alcohol and contact lenses do not mix.
Patients are not required or encouraged to wear gloves. If they want to, that is fine.
What’s next?
Now that you have a safety plan for the people in your practice, you need to turn your attention to the facility itself. Next time we will talk about the physical changes you need to make for the health and safety of your patients and employees.
Remember to take some time for yourself and bolster your optical knowledge with our CEs, many of which are free, courtesy of educational grants from our sponsors at 2020mag.com/ce.











