By Barry Santini
Does this sound familiar, except for the apparently misspelled company’s name?
For Immediate Release:
“The most advanced technology for presbyopic eyeglass wearers is found in the developments of progressive lens design. Unlike traditional single vision, bifocal and trifocal lenses, progressive lenses demand greater degrees of accuracy and precision in both measurements and fitting in order to fully enjoy and realize their advantages and performance. To help facilitate, educate and advance eyecare professionals to the goal of obtaining measurements that are not only more accurate, but also more precise and more repeatable, Essel of France has developed a new type of instrument that takes a photo of the patient while wearing their chosen frame. This photo-based method promises to reduce error and improve accuracy in both pupillary distance as well as eyepupil height measurements.”
You might be surprised to learn that this fictitious press release could have accompanied the introduction of an instrument called Centromatic, in 1972—nearly 40 years ago. The Centromatic, developed by one of Essilor’s parent companies, was the first commercial picture-taking instrument designed to improve accuracy and repeatability in eyewear measurements. It was intended to be used when fitting the first and second generation of Varilux progressive lenses. It’s amazing not only how closely the Centromatic resembles some of today’s digitally based models, but also the apparent similarity to the challenges facing eyecare professionals with today’s latest digitally surfaced, free-form manufactured and position-of-wear compensation progressive, wrap and single vision lenses.
While many ECPs have felt that although PDs are essential for proper eyewear fabrication, there is not general agreement as to the precision of the measurement, or the methodology that should be used. From the familiarity of the basic PD stick, to the “oh, my gosh,” 2001-like apparition of the newer digital centration devices, it may be time to take a look at the various viewpoints and even battle lines that are developing now for your patient’s PD.
Why Take a PD Anyway?
With the broad availability of pre-made, over-the-counter magnifier/reading glasses, as well as sunglasses featuring “magnifying” bifocal areas, a case can be made that simply fabricating most prescriptions under four diopters to a reasonable “eyeball” estimate of a customer’s binocular pupillary distance should be sufficiently accurate to ensure a lack of permanent harm to one’s vision. As an eyecare professional, trained, certified and trusted with the responsibility for ensuring the best for your patient’s eyes, you recognize this argument is overly simplistic. Unfortunately, the public does not. Simply defining the threshold of acceptable risk of harm to one’s vision as only the point where uncorrectable or sustained visual impairment has occurred totally misses the point of our education and training as eyecare professionals, don’t you think?
What Harm Can an Incorrect PD Cause?
Over 90 percent of the sensory information we process is taken in through our eyes. The greatest threat of harm that we’re exposed to in our daily lives connected with vision is driving. During driving, vision is clearly the most important and essential sense that’s required to be performing at its best in order to avoid accidental harm to ourselves and others. As eyecare professionals, it is therefore our desire and mandate to deliver the best possible visual performance to each and every person who walks into our office. The health of both individuals and society is at stake. Although an improperly made PD will rarely cause permanent harm to one’s vision, it certainly can affect depth perception, judgment of distance and contrast sensitivity—all factors known to influence driving safety.
The Battle for Your PD
With the broad arrival of prescription eyewear over the Internet, a turf war has broken out over who actually “possesses” the patient’s PD— the ECP or the patient? We won’t enter this debate here, but we will recognize that digital photo technology is allowing web sites to declare that they can determine your PD as accurately—or sometimes even more accurately—from the eye measurements gleaned from the customer’s uploaded photo. The implication to the consumer is that their eyecare professional is falling behind the times when they continue using a PD stick or pupillometer. If your patient believes they can realize the promise of an accurate pupillary measurement from a photo they’ve taken themselves, why should an ECP be concerned with maintaining their PD supremacy through an investment in digital centration technology, when ink-stained rulers and make-up encrusted pupillometers have apparently done the job satisfactorily up to now?
This argument may appear overly simplistic to some of us in the industry. Yet, we really need to recognize that we’re enmeshed in a paradigmic change in the way in which consumers choose to buy any type of goods today, whether it is shoes, appliances or, yes, prescription eyewear. How you as the eyecare professional obtain and explain the importance of this measurement as a high precision and personal experience for your customers is essential to containing the doubts your patients might have about your relevance to their eyewear purchases. At a minimum, your relevance to their eyewear selection and purchase should no longer to be taken for granted. It’s a new world out there, and we ECPs better wake up to this fact fast, before we become Rumplestilskins ourselves.
The Battle for Your PD
With the broad arrival of prescription eyewear over the Internet, a turf war has broken out over who actually “possesses” the patient’s PD— the ECP or the patient? We won’t enter this debate here, but we will recognize that digital photo technology is allowing web sites to declare that they can determine your PD as accurately—or sometimes even more accurately—from the eye measurements gleaned from the customer’s uploaded photo. The implication to the consumer is that their eyecare professional is falling behind the times when they continue using a PD stick or pupillometer. If your patient believes they can realize the promise of an accurate pupillary measurement from a photo they’ve taken themselves, why should an ECP be concerned with maintaining their PD supremacy through an investment in digital centration technology, when ink-stained rulers and make-up encrusted pupillometers have apparently done the job satisfactorily up to now?
This argument may appear overly simplistic to some of us in the industry. Yet, we really need to recognize that we’re enmeshed in a paradigmic change in the way in which consumers choose to buy any type of goods today, whether it is shoes, appliances or, yes, prescription eyewear. How you as the eyecare professional obtain and explain the importance of this measurement as a high precision and personal experience for your customers is essential to containing the doubts your patients might have about your relevance to their eyewear purchases. At a minimum, your relevance to their eyewear selection and purchase should no longer to be taken for granted. It’s a new world out there, and we ECPs better wake up to this fact fast, before we become Rumplestilskins ourselves.
Why Pictures for PDs?
Did you grow up with the millimeter ruler as a familiar and essential part of your dispensing toolbox? I did. But it is the very comfortable and familiar need to reach for a ruler when taking measurements that must be challenged to begin to realize the most from today’s advanced digitally surfaced lenses. Using simple binocular measurements and/or overlooking the need for taking monocular pupil heights for every pair of eyewear will diminish your patient’s enjoyment of these advanced and expensive lenses. They will also, most importantly, shortchange your client from experiencing how your practice is advancing into the 21st century as well.
Let’s review the advantages of taking the more typical eyewear measurements through the magic of a digital photograph:
- Precision is enhanced—Most digital devices deliver a precision of a tenth of a millimeter, which is more precise by a factor of five than a common digital-readout pupillometer.
- Accuracy is enhanced—With parallax correcting algorithms, digital centration equipment can compare the cardinal points of the “Frame Reference Device” (an attachment placed on the patient’s eyewear before the picture is taken) with known reference values for the same and correct for left-right and up-down deviations in patient head posture. Some units even display the value of the deviational error for the practitioner’s reference.
- Repeatability is enhanced—In many busy offices, there are multiple employees of varying skill levels. Digital picture measurements reduce the variations between operators as well as between successive measurements by a single operator.
- Frame fit is properly considered—With rulers and even pupillometers, the manner in which a frame may sit, whether for comfort, aesthetics or personal patient preference, has never been part of the measuring process. Digital picture measurements ensure much greater accuracy, as they integrate the above factors seamlessly into the final measured values.
- Position of Wear values are easily obtained—The advent of wrap around eyewear, as well as position of wear enhanced single vision and progressive lenses, require that ECPs obtain good values not only for PD and pupil height, but also for vertex distance, pantoscopic tilt and panoramic (aka face-form) angle. Taking these measurements can be daunting to dispensary personal, primarily due to their unfamiliarity. Obtaining these via digital pictures is easy and makes both dispensary and lab better partners in the visual performance delivered to the patient.
The Absolute Latest in Technology
All of the current digital measurement-via-picture devices include the following items:
- Integrated Video Camera and Screen for display—With these two items, these become more than measuring instruments. They represent the current state of the art for in-office, patient frame-try-on capability. All feature good image resolution and natural color rendition. Note: Most units do not attempt to deliver HD images. Because of the intimate, close-up nature of the facial images, field experience has revealed that patients prefer not seeing certain aspects of their face and skin rendered in extra fine, high-definition detail, for all around to see. The screens images therefore attempt to strike a good compromise between rendering the face accurately and not acting as a magnifying display for real or perceived flaws.
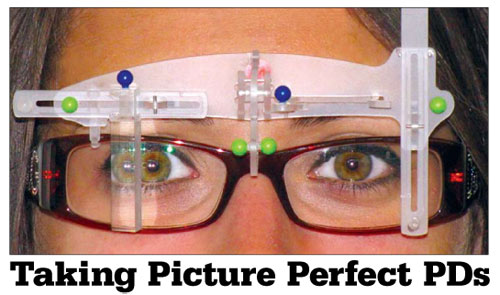
- Frame Reference Device—In order to provide the proper cardinal reference for taking truly precise and accurate measurements, all systems attach a Frame Reference Device to the chosen frame. Depending upon the system chosen, a machine-derived measurement of frame and pupil position is first obtained. The ECP can then tweak and adjust the cardinal points to ensure they have been properly obtained and registered, which further improves precision and accuracy.
- Archiving the picture and measurements—After the photo is taken, wonderful choices are available to the ECP in the next step:
- a. Store the image/info file on an attached disk or flash drive for later retrieval.
- b. Print the image/info out to an attached or wireless printer.
- c. Email the image/info directly to your lab to tag along with an eyewear order.
- d. Integrate the image/photo into your practice management software for later retrieval, or to forward onto your lab through your favorite online ordering portal.
- Demonstration of tints, photochromics, polarizing lenses and AR coatings—These options can be overlaid onto the selected frame style, including adjustments to hue and density. Photochromic lenses, including specific brands, can be selected. Examples include such popular options as Drivewear, Transitions and polarizing lenses.
- Rendering and demonstration of finished thickness with different lens materials—By typing in the patient’s Rx and selecting the material index, a three-dimensional representation of the finished lens profile thickness is shown, customized to the chosen frame size and shape.
- Vision Screening—including basic acuity and color blindness tests.
- Demonstration of contact lenses—Some models may utilize some of the above features in demonstrating various contact lens tints.
- General Presentations—Generic or manufacturer-specific lens demonstrations may be available for user-upload. Units may also be configured for a default screen-saver and the ECP may choose a polarization presentation to appear continuously while the unit is unattended.
Wrong. Whether you choose to lease or finance, most systems easily pay for themselves through the sale of just two pairs of free form progressive lenses per month.
A Picture Worth a Thousand Words
Today, you can use a variety of media to advertise your business: radio, print, direct mail and the web. But nothing will ever beat the power that “word-of-mouth” from present clients does in driving new patients to your office. And every new client represents the opportunity to build a lifelong relationship. Further, nothing impresses a client as much as an office that adopts, uses and demonstrates their commitment to the state-of-the-art in advancements of vision care.
The old saying remains: One picture is worth a thousand words. Get started with digital centration today. The last thing you’ll want your office’s vision care to appear is behind the web when it comes to adopting the advantage of digital pictures.
Barry Santini is a New York State licensed optician base in Seaford, N.Y.













