Since refractive surgery achieved widespread use in the 1980s with radial keratotomy, patients and physicians alike have wondered about the comparative safety of refractive surgery vs. contact lenses. The reason the debate has never been laid to rest lies in the difficulty of comparing the two modalities' risks: with contact lenses, patients assume a certain amount of risk each year; while with refractive surgery most of the risk occurs at the time of surgery. This article will look at the research on the topic and arguments from both sides.
A Challenging Comparison
Physicians and researchers say that one of the central difficulties in comparing contact lens wear to refractive surgery in terms of safety is that the two modalities address the refractive error in very different ways.
Tijuana
"With contact lenses, however, you have an inverted safety curve," Dr. Chayet continues. "This means the first day the patient starts using contact lenses, the risk is minimal. Then, the risk starts to build and there's an increased risk of developing a sight-threatening keratitis with time."
Currently, the two sides of the debate compare the two vision-correction methods in terms of the risk of losing best-corrected vision, usually from a corneal ulcer in the case of lenses, since that's an adverse event that both have in common. Contact lens proponents, however, think vision quality should be considered, too.
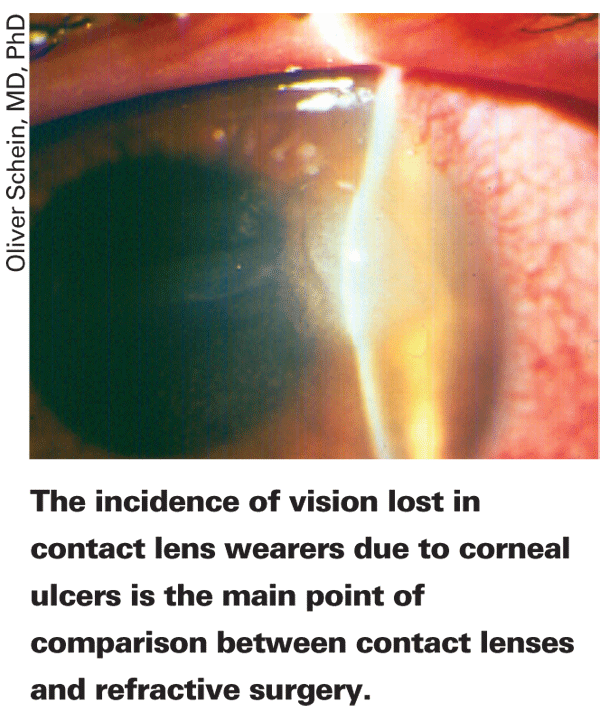
"With contact lenses, the only thing that may cause scarring and decreased vision is infection," says Wilmer Eye Institute's Oliver Schein, MD. "For refractive surgery, the primary concern is those who lose one or more lines of best-corrected vision, but that's not sufficient. There are clearly patients who lose no lines or one line but who complain bitterly about the quality of their vision. There aren't many of these patients, since refractive surgery typically gets satisfaction rates in the high 90-percent range. However, if 4 or 5 percent of patients aren't satisfied with their vision following refractive surgery, that's more than the number who suffer from decreased vision due to an ulcer from contact lens wear." And, the contact-lens trump card is that wearers can always stop wearing their lenses.
William Mathers, MD, of the Casey Eye Institute at the Oregon Health and
"Of course, you also have to compare the problems of people who have refractive surgery for modest visual impairment," Dr. Mathers continues. "When you get over about -9 D or-10 D, you enter a different category, in my opinion. Over -10 D, most people are better with contact lenses. If they can't wear contact lenses, they might be better off with something like a phakic intraocular lens or even refractive lensectomy."
Comparing Studies
When the debate is focused on loss of vision, the two camps find it difficult to agree on which studies are eligible for comparison, which again highlights the differences inherent in the modalities. The contact-lens side says it has multiple large-scale, population-based studies with thousands of wearers to use for analysis of incidences of complications such as corneal ulcers,1 while refractive surgery studies are smaller and lack the same statistical power.
"The latest key contact-lens paper is from Fiona Stapleton, PhD, in
Dr. Schein feels similarly. "The remarkable thing is that, if you look at the large contact lens studies, they all get pretty much the same result in terms of infection rates," he says. "They're very strong studies because they're population-based. This means that when you determine a rate of infection with contact lenses in the study, it's based on a large community with all providers and users included. But all of the LASIK literature comes from individual surgeons, a practice or a center or two that got together to report their results. They're only talking about their own patients."
Dr. Mathers, however, thinks a population-based LASIK study isn't impossible. "It would be reasonable to do that," he says. "It doesn't have to be done in the
Comparing the Risks
Though there's data regarding the incidence of microbial keratitis in large populations of contact lens wearers, the challenge comes when one tries to come up with an individual lens-wearer's risk of getting a sight-threatening ulcer in his lifetime.
The contact-lens study from
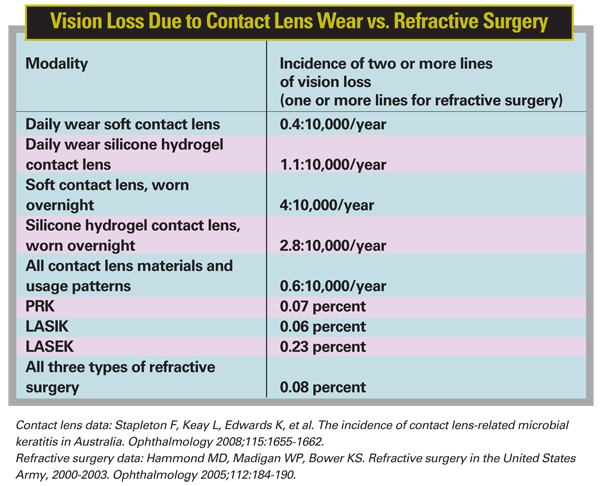
Ultimately, Dr. Stapleton's study determined that there's an annual incidence of 0.6 cases that lose two or more lines of best-corrected vision per 10,000 contact wearers.2 The study found that the riskiest type of use was overnight wear: Overnight wearers of soft lenses were 10 times more likely to have a sight-threatening ulcer than daily-wear soft lens users.
In the absence of a population-based study, Dr. Mathers puts stock in the large retrospective refractive surgery study performed by the U.S. Army between 2000 and 2003.3 The study analyzed the results of 32,068 eyes of 16,111 soldiers who underwent PRK (n=20,745 eyes), LASIK (n=8,528 eyes) or LASEK (n=2,795 eyes). Not all patients had both eyes done. With a follow-up of at least three months, 0.08 percent lost one or more lines of vision.
Incidences of lost vision for both contacts and refractive surgery from the two studies appear in Table 1.
However, just knowing these incidences isn't enough, say proponents of refractive surgery. To get at contact lenses' true risk, you need to extrapolate the risk over decades. That's where the debate takes another turn.
In short, supporters of refractive surgery feel you should calculate the risk of contact lens wear in such a way that it accumulates over time, building to a greater overall risk when all the years are taken into account. Dr. Mathers is currently composing an article on the topic and, though he can't share specific numbers or his calculations, he's concluded that the risk of losing vision by wearing extended wear contact lenses exceeds that of laser surgery within a couple of years. He adds that soft lenses' are much less risky than extended wear, and that rigid-gas permeable lenses are the safest, taking several decades to become riskier than laser surgery.
Dr. Schein, however, says calculating the odds of getting a sight-threatening infection isn't that simple. "The rate isn't the same every year," he says. "If I was born yesterday, for example, there are actuarial tables to tell me the likelihood of living to age 75. Now, if you talk to me at age 53, and I've been fortunate enough to not have had any major illnesses, my likelihood of reaching age 75 is much higher than at birth, because I've already survived the past 53 years and I'm healthy. So, if I start wearing extended wear lenses tomorrow and it's two years from now and I haven't gotten an ulcer, my risk isn't going up or staying the same—it's going down. This is because I've already shown that I'm a survivor because of the way I take care of the lenses, the organisms on my lid or other factors."
In actuality, both sides may be right. Ophthalmologist Nathaniel Knox Cartwright, MRCOphth, of the
Ultimately, the choice of which modality is better for a patient comes down to the joint decision of a patient and his physician, as both lens wear and refractive surgery are safe in properly selected individuals.
"I do many refractive laser procedures, and I'm also president-elect of the International Society of Contact Lens Research," says Dr. Cavanagh. "I think both contacts and laser surgery are extraordinary options. When you get down to risks of 1:5,000 or 1:20,000 of sight-threatening infections, you're getting down around the risk of injury in a car while wearing a safety belt. When you get down to these low numbers, it becomes a distinction without a difference."
1. Poggio EC, Glynn RJ, Schein OD, et al. The incidence of ulcerative keratitis among users of daily-wear and extended-wear soft contact lenses. N Engl J Med 1989 21;321:12:779-83.
2. Stapleton F, Keay L, Edwards K, et al. The incidence of contact lens-related microbial keratitis in
3.
4. Ren DH, Yamamoto K, Ladage PM, et al. Adaptive effects of 30-night wear of hyper-O(2) transmissible contact lenses on bacterial binding and corneal epithelium: A 1-year clinical trial. Ophthalmology 2002;109:27-39.











